When your kidneys struggle to filter waste from your blood, the impact ripples through your entire body. But what happens when this condition isn’t just a random health event—when it’s written into your very genes? For millions of families worldwide, kidney disease isn’t just a medical diagnosis; it’s a shared legacy passed down through generations.
Many people discover they have kidney problems only after significant damage has occurred, unaware that their family history placed them at heightened risk from birth.
Without understanding the genetic connections, families miss crucial opportunities for early testing and intervention, potentially watching multiple generations face dialysis or transplant.
Learning about hereditary kidney disease empowers you to take control of your health destiny through informed decisions about testing, monitoring, and management.
Understanding the genetic factors behind kidney conditions represents one of the most important steps in protecting your health and that of your loved ones. Let’s explore how hereditary kidney disorders develop, what symptoms to watch for, and how modern medicine offers hope for managing these inherited conditions.
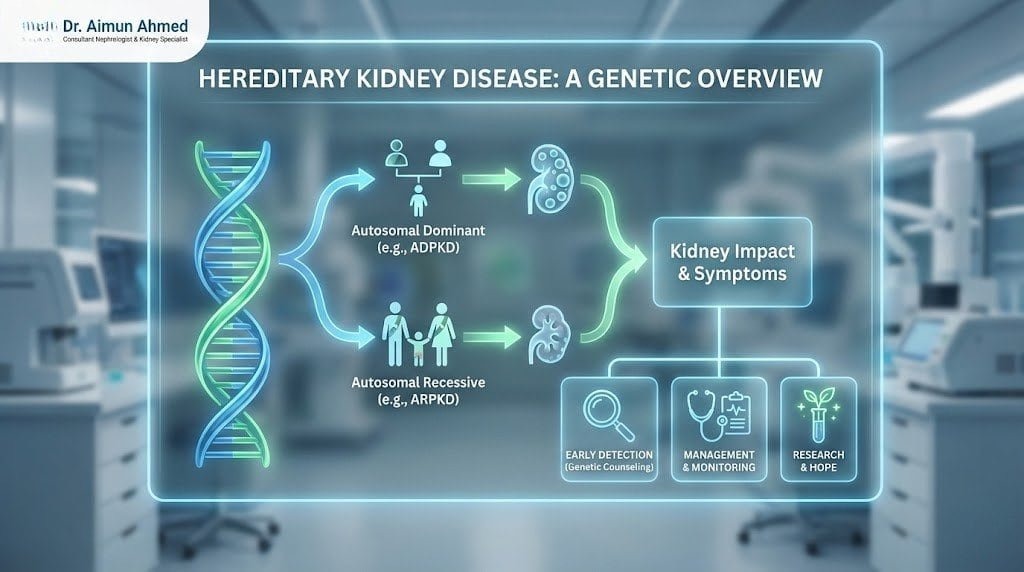
Does Kidney Disease Run in Families?
The short answer is yes—many kidney diseases have strong genetic components that make them more likely to appear across multiple family members. When we talk about hereditary kidney diseases, we’re discussing conditions where specific gene mutations or variations increase your likelihood of developing kidney problems.
Research shows that if you have a parent with chronic kidney disease, your risk of developing similar issues increases significantly compared to the general population. This connection happens because certain genetic mutations affect how your kidneys develop, function, and respond to environmental factors throughout your lifetime.
Key Risk Factors for Hereditary Kidney Disease:
- Having a parent or sibling with diagnosed kidney disease increases your risk by 2-3 times
- Multiple family members with kidney problems suggest stronger genetic links
- Early-onset kidney disease in relatives (before age 50) indicates higher hereditary risk
- Family history of conditions like diabetes or high blood pressure that damage kidneys
- Ethnic background plays a role, with some populations having higher rates of certain genetic kidney disorders
However, family history doesn’t guarantee you’ll develop kidney disease. Genetics represents just one piece of a complex puzzle that includes lifestyle choices, environmental exposures, and other health conditions like diabetes and heart disease.
Understanding Genetic Kidney Conditions
Genetic conditions affecting the kidneys encompass a wide range of disorders, from common hereditary kidney diseases to extremely rare kidney disease that is hereditary in nature. These conditions result from mutations in specific genes that control kidney development, structure, or function.
Some genetic kidney disorders appear at birth, while others don’t show symptoms until adulthood. The timing depends on the specific gene involved and how the mutation affects kidney function over time.
How Genetic Mutations Affect Kidneys:
- Structural defects: Genes controlling kidney development can cause abnormal kidney shape or size
- Filtering problems: Mutations may damage the kidney’s filtering units (nephrons)
- Cyst formation: Certain genes trigger fluid-filled sacs that enlarge kidneys and reduce function
- Protein abnormalities: Defective genes produce faulty proteins needed for kidney cell structure
- Metabolic disorders: Some mutations prevent kidneys from processing specific substances properly
Researchers have identified hundreds of genes associated with kidney disease risk, and this knowledge continues to grow as genome studies advance. Mount Sinai and other leading medical institutions have made significant contributions to understanding how genetic mutations lead to kidney damage. This knowledge helps doctors provide more accurate diagnoses and develop targeted therapies for patients with inherited kidney conditions.
Polycystic Kidney Disease: The most common kidney hereditary condition
Polycystic kidney disease (PKD) stands as the most common genetic disorder of the kidney, affecting approximately 1 in 500 to 1,000 people worldwide. This condition causes numerous cysts to grow in the kidneys, making them bigger over time and gradually reducing their ability to function properly.
Types of Polycystic Kidney Disease:
- Autosomal Dominant PKD (ADPKD): The most common form, usually appearing in adulthood between ages 30-50. If one parent has ADPKD, each child has a 50% chance of inheriting it.
- Autosomal Recessive PKD (ARPKD): Much rarer, typically affecting infants and children. Both parents must carry the gene mutation for a child to develop this form.
Common complications of PKD:
- High blood pressure develops in about 60% of patients before kidney function declines
- Kidney stones affect approximately 20% of people with PKD
- Urinary tract infections occur more frequently due to cyst formation
- Liver cysts develop in about 80% of adults with ADPKD, though rarely cause problems
- Heart valve abnormalities appear in some patients
- Brain aneurysms occur in 5-10% of PKD patients, requiring screening in high-risk families
The disease’s progression varies significantly between individuals, even within the same family. Some people maintain relatively healthy kidney function well into their 60s or 70s, while others develop end-stage renal disease (ESRD) requiring dialysis or transplant in their 40s or 50s.
Rare kidney disease that is hereditary
Beyond PKD, several rare kidney conditions follow hereditary patterns. Alport Syndrome affects the body’s collagen production, damaging the tiny filters in your kidneys called nephrons. This disorder often affects hearing and vision alongside kidney function.
Characteristics of Alport Syndrome:
- Progressive hearing loss, typically beginning in childhood or adolescence
- Eye abnormalities including lens problems and retinal changes
- Blood in urine (hematuria) from early childhood
- Protein in urine that worsens over time
- Kidney failure typically develops in males during their 20s-30s
- Females with the mutation usually have milder symptoms
Fabry disease represents another rare genetic kidney disease where the body cannot break down certain fatty substances, leading to their accumulation in cells throughout the body, including the kidneys. Early diagnosis and enzyme replacement treatments can slow disease progression significantly.
Other Rare Hereditary Kidney Disorders Include:
- Cystinosis: Abnormal cystine crystal accumulation in kidney cells
- Primary Hyperoxaluria: Excessive oxalate production leading to kidney stones
- Dent Disease: X-linked disorder causing protein loss and kidney stones
- Nail-Patella Syndrome: Affects nails, knees, elbows, and kidneys
- Congenital Nephrotic Syndrome: Severe protein loss beginning in infancy
Each condition presents unique challenges and requires specialized care from experienced nephrologists.
Hereditary kidney disease symptoms
Recognizing hereditary kidney disease symptoms early makes a tremendous difference in treatment outcomes. Unfortunately, kidneys are remarkably efficient at compensating for damage, meaning symptoms often don’t appear until significant function has been lost.
Early Warning Signs of Kidney Disease:
- Changes in urination: Increased frequency (especially at night), decreased amount, dark or bloody urine, excessive foaming
- Persistent fatigue: Feeling exhausted despite adequate sleep, as kidneys fail to remove toxins and produce energy-regulating hormones
- Swelling (edema): Puffiness around eyes in the morning, swollen ankles and feet, especially noticeable in the evening
Progressive symptoms as disease advances:
- Shortness of breath from fluid buildup in lungs
- Nausea and vomiting due to waste accumulation
- Loss of appetite and unintended weight loss
- Muscle cramps, particularly in legs
- Difficulty concentrating and memory problems
- Persistent itching across the body
- Metallic taste in mouth and bad breath
- Sleep disturbances and restless legs
Symptoms specific to certain hereditary conditions:
- PKD symptoms: Back or side pain from enlarged kidneys, frequent urinary tract infections, blood in urine
- Alport syndrome: Hearing loss in childhood, vision problems, blood in urine from early age
- Fabry disease: Burning pain in hands and feet, skin rash, heat intolerance, gastrointestinal problems
Blood in urine or foamy urine can indicate protein leakage, a key sign of kidney damage. For specific conditions like PKD, people might experience pain in the back or sides as enlarged kidneys press against surrounding organs.
Hereditary kidney disease list
Understanding the full spectrum of hereditary kidney diseases helps families recognize their potential risks. Here’s a comprehensive breakdown of genetic kidney disorders:
Common Hereditary Kidney Disorders:
- Polycystic Kidney Disease (PKD): Multiple cysts causing kidney enlargement and function loss
- Alport Syndrome: Collagen defect affecting kidneys, ears, and eyes
- Thin Basement Membrane Nephropathy: Mild haematuria with generally good prognosis
- Medullary Cystic Kidney Disease: Cysts in kidney’s inner region leading to scarring
- Fabry Disease: Enzyme deficiency causing fatty substance accumulation
Rare Genetic Kidney Conditions:
- Primary Hyperoxaluria: Overproduction of oxalate causing stones and kidney damage
- Cystinosis: Cystine crystal buildup in kidneys and other organs
- Dent Disease: Tubular disorder causing stone formation and protein loss
- Nail-Patella Syndrome: Skeletal abnormalities combined with kidney disease
- Congenital Nephrotic Syndrome: Early-onset severe protein loss
- Bartter Syndrome: Salt-wasting disorder affecting electrolyte balance
- Gitelman Syndrome: Magnesium and potassium wasting condition
Metabolic disorders affecting kidneys:
- Cystinuria (excessive cystine causing stones)
- Primary hyperoxaluria types 1, 2, and 3
- Adenine phosphoribosyltransferase deficiency
- Hereditary renal hypouricemia
This list represents just a fraction of genetic kidney disorders researchers have identified. Each condition has distinct characteristics, inheritance patterns, and treatment approaches.
Is Stage 3 Kidney Disease Hereditary?
Stage 3 chronic kidney disease describes a level of kidney function rather than a specific hereditary condition. However, the underlying cause of Stage 3 kidney disease can certainly be hereditary.
Understanding kidney disease stages:
- Stage 1: Normal or high kidney function (GFR ≥90) with kidney damage
- Stage 2: Mild reduction in function (GFR 60-89) with kidney damage
- Stage 3a: Mild to moderate reduction (GFR 45-59)
- Stage 3b: Moderate to severe reduction (GFR 30-44)
- Stage 4: Severe reduction (GFR 15-29)
- Stage 5: Kidney failure (GFR <15 or on dialysis)
If your Stage 3 kidney disease results from conditions like PKD, Alport syndrome, or other genetic disorders, then yes, the root cause is hereditary. However, if your kidney disease stems from diabetes, high blood pressure, or other non-genetic factors, the Stage 3 classification itself isn’t inherited—though your family may share risk factors for these conditions.
When stage 3 kidney disease may be hereditary:
- Diagnosed before age 50 without clear non-genetic causes
- Family members with similar kidney problems at comparable ages
- Presence of genetic markers or mutations in testing
- Associated symptoms suggesting hereditary conditions (hearing loss, cysts, skin problems)
- Multiple affected relatives across generations
Understanding this distinction matters because it affects screening recommendations for your relatives.
List of rare kidney diseases
Rare kidney diseases often go undiagnosed for years because doctors may not immediately consider uncommon conditions. Understanding these disorders helps patients and families recognize potential symptoms earlier.
Rare Tubular disorders:
- Bartter Syndrome: Affects salt reabsorption, causing low potassium, low blood pressure, and excessive urination. Symptoms include muscle weakness, cramping, and growth delays in children.
- Gitelman Syndrome: Similar to Bartter but typically appears later with milder symptoms. Patients experience fatigue, muscle cramps, salt cravings, and low magnesium.
- Fanconi Syndrome: Multiple tubular defects causing loss of glucose, amino acids, phosphate, and other substances in urine.
Rare cystic kidney diseases:
- Nephronophthisis: Group of inherited disorders causing cysts and leading to ESRD, often during childhood or adolescence. The most common genetic cause of kidney failure in children.
- Medullary Sponge Kidney: Cystic dilation of collecting ducts, often discovered incidentally, may cause stones and infections.
Rare kidney inflammatory conditions:
- IgA Nephropathy: While more common than other rare diseases, still represents a significant autoimmune cause of kidney failure where immune complexes attack kidney tissues.
- C3 Glomerulopathy: Rare disorder of complement system causing kidney inflammation.
Genetic metabolic disorders:
- Cystinuria: Hereditary disorder causing cystine stones
- Primary hyperoxaluria: Liver enzyme defects causing oxalate overproduction
- Adenine phosphoribosyltransferase deficiency: Causes 2,8-dihydroxyadenine stone formation
Rare kidney disease symptoms
Rare kidney conditions often present with symptoms that overlap with more common kidney diseases, making diagnosis challenging. However, certain patterns can suggest specific rare disorders.
General symptoms suggesting rare kidney disease:
- Kidney problems beginning in childhood or adolescence
- Unusual urine findings (crystals, excessive protein, glucose despite normal blood sugar)
- Recurrent kidney stones, especially in children or young adults
- Kidney disease combined with symptoms in other body systems
- Poor response to standard kidney disease treatments
- Family history of unexplained kidney problems
Symptoms pointing to specific rare conditions:
Tubular Disorders (Bartter, Gitelman, Fanconi):
- Excessive thirst and urination
- Salt cravings
- Muscle weakness and cramping
- Growth delays in children
- Low blood pressure despite kidney disease
- Bone problems from mineral imbalances
Fabry Disease:
- Burning pain in hands and feet (acroparesthesias)
- Distinctive skin lesions (angiokeratomas)
- Heat intolerance and inability to sweat properly
- Gastrointestinal problems
- Heart rhythm abnormalities
- Stroke risk in young adults
Metabolic stone disease:
- Recurrent kidney stones beginning in childhood
- Kidney calcification visible on imaging
- Urinary tract infections
- Blood in urine
- Abdominal or flank pain
Alport Syndrome:
- Hearing loss progressing through childhood
- Eye problems (lens abnormalities, retinal changes)
- Blood in urine from infancy
- Progressive kidney function decline
Some rare kidney diseases cause symptoms in other body systems, explaining why doctors must consider the whole person when evaluating potential hereditary kidney disorders.
Genetic Kidney disease treatment
Treatment for genetic kidney disease has advanced remarkably in recent decades. While we cannot yet cure most hereditary kidney diseases, we can significantly slow progression and manage symptoms through targeted therapies.
General treatment approaches for hereditary kidney disease:
Blood Pressure Management:
- ACE inhibitors or ARBs as first-line medications to protect kidney function
- Target blood pressure below 130/80 mmHg for most patients
- More aggressive control (below 120/80) may benefit some with heavy proteinuria
- Regular home monitoring to ensure consistent control
Dietary modifications:
- Reduced sodium intake (less than 2,300 mg daily, ideally 1,500 mg)
- Protein restriction in advanced stages (0.6-0.8 g/kg body weight)
- Potassium and phosphorus limitations as kidney function declines
- Adequate fluid intake unless fluid restriction needed
- Mediterranean or DASH diet patterns support kidney health
Lifestyle interventions:
- Regular exercise (30 minutes most days) improves blood pressure and overall health
- Smoking cessation prevents accelerated kidney damage
- Maintaining healthy weight reduces strain on kidneys
- Avoiding nephrotoxic substances (certain painkillers, herbal supplements)
- Stress management through meditation, yoga, or counseling
Specific treatments for individual conditions:
Polycystic Kidney Disease:
- Tolvaptan (Jynarque) slows cyst growth and preserves kidney function in rapidly progressing ADPKD
- Aggressive blood pressure control particularly important
- Pain management for cyst-related discomfort
- Prompt treatment of infections
- Avoiding caffeine may help slow cyst growth
Alport Syndrome:
- Early use of ACE inhibitors or ARBs before significant proteinuria develops
- Hearing aids for progressive hearing loss
- Eye care for vision problems
- Avoiding contact sports to prevent hearing damage
Fabry Disease:
- Enzyme replacement therapy (agalsidase alfa or beta) administered every two weeks
- Chaperone therapy (migalastat) for patients with specific mutations
- Pain medications for neuropathic pain
- Heart medications for cardiac complications
Rare Metabolic disorders:
- Pyridoxine (vitamin B6) for certain types of primary hyperoxaluria
- High fluid intake for stone-forming conditions
- Specific dietary restrictions based on metabolic defect
- Medications to alkalinize urine in some stone diseases
Advanced treatment options:
When Kidney Function Declines:
- Dialysis (hemodialysis or peritoneal dialysis) when GFR drops below 15
- Kidney transplantation offers best outcomes for eligible patients
- Living donor transplants provide superior long-term results
- Some genetic conditions may recur in transplanted kidney, requiring specific considerations
Emerging Therapies:
- Gene therapy research shows promise for correcting genetic defects
- CRISPR technology being explored for genetic kidney diseases
- New targeted medications in clinical trials for various hereditary conditions
- Precision medicine approaches based on individual genetic profiles
Comprehensive care extends beyond medications. Regular monitoring allows doctors to adjust treatments as the disease progresses, ensuring optimal outcomes at every stage.
While autoimmune kidney disease isn’t strictly hereditary, genetic factors influence who develops these conditions. In autoimmune disorders, the immune system mistakenly attacks healthy kidney tissues, causing inflammation and damage.
Common Autoimmune Kidney Conditions:
Lupus Nephritis:
- Kidney inflammation from systemic lupus erythematosus (SLE)
- Affects about 50% of lupus patients
- Symptoms include foamy urine, swelling, high blood pressure
- Treated with immunosuppressive medications like cyclophosphamide or mycophenolate
IgA Nephropathy:
- Most common primary glomerular disease worldwide
- IgA antibodies deposit in kidney filters
- Often presents with blood in urine during infections
- Treatment includes blood pressure control, fish oil, and immunosuppression in severe cases
Anti-GBM Disease (Goodpasture Syndrome):
- Antibodies attack kidney and lung basement membranes
- Requires urgent treatment with plasmapheresis and immunosuppression
- Can cause rapid kidney failure without prompt intervention
ANCA-Associated Vasculitis:
- Includes granulomatosis with polyangiitis and microscopic polyangiitis
- Small blood vessel inflammation affects kidneys and other organs
- Treatment involves high-dose steroids and medications like cyclophosphamide or rituximab
Genetic Factors in autoimmune kidney disease:
- Certain HLA gene variants increase risk for lupus and other autoimmune conditions
- Family members of autoimmune disease patients have higher risk
- Multiple genes influence immune system function and self-tolerance
- Environmental triggers combine with genetic predisposition to cause disease
- Ethnic background affects risk (lupus more common in African, Hispanic, and Asian populations)
Treatment typically involves immunosuppressive medications to calm the overactive immune response. Early intervention improves outcomes significantly, making prompt diagnosis crucial for preserving kidney function.
Testing and diagnosis: your path forward
How to test for genetic kidney disease depends on your symptoms, family history, and which conditions doctors suspect. Comprehensive evaluation combines multiple testing approaches for accurate diagnosis.
Basic Kidney Function Tests:
Blood Tests:
- Serum creatinine measures waste product levels
- Estimated glomerular filtration rate (eGFR) calculates kidney filtering capacity
- Blood urea nitrogen (BUN) assesses waste removal
- Electrolytes (sodium, potassium, phosphorus, calcium) check mineral balance
- Complete blood count detects anemia common in kidney disease
Urine Tests:
- Urinalysis screens for protein, blood, glucose, and infection
- Urine protein-to-creatinine ratio quantifies protein leakage
- 24-hour urine collection measures total protein and creatinine clearance
- Urine microscopy identifies cells, casts, and crystals
Imaging studies:
Ultrasound:
- First-line imaging showing kidney size, shape, and cysts
- Non-invasive with no radiation exposure
- Can detect PKD, obstruction, and structural abnormalities
- Doppler ultrasound assesses blood flow to kidneys
CT Scan:
- Detailed images revealing cysts, stones, and masses
- Better visualization than ultrasound for complex cases
- Contrast CT provides additional information but requires good kidney function
MRI:
- Excellent soft tissue detail without radiation
- Useful for evaluating masses and vascular problems
- MRA (angiography) visualizes kidney blood vessels
- Can measure kidney volume in PKD monitoring
Genetic testing:
When Genetic Testing Is Recommended:
- Family history of hereditary kidney disease
- Early-onset kidney disease (before age 50) without clear cause
- Kidney disease with extra-renal symptoms (hearing loss, vision problems, skin changes)
- Multiple family members affected across generations
- Planning pregnancy with known genetic kidney disease in family
- Unexplained kidney disease in children
Types of genetic gests:
Single Gene Testing:
- Targets specific genes when clinical features suggest particular condition
- Used when diagnosis is relatively certain (e.g., PKD with family history)
- Faster and less expensive than comprehensive testing
Gene Panel Testing:
- Tests multiple genes simultaneously
- Useful when several conditions are possible
- Kidney disease panels may include 50-300 genes
- Increases likelihood of finding causative mutation
Whole Exome Sequencing:
- Analyzes all protein-coding genes (about 20,000 genes)
- Used when panels don’t reveal diagnosis
- May discover new or ultra-rare genetic causes
- Requires expert interpretation
Whole Genome Sequencing:
- Most comprehensive, analyzing entire DNA sequence
- Currently used primarily in research
- May become more common as costs decrease
Kidney Biopsy
Sometimes needed for definitive diagnosis, especially when:
- Cause of kidney disease remains unclear
- Treatment decisions depend on specific kidney changes
- Distinguishing between different types of glomerular disease
- Assessing disease severity and guiding treatment intensity
Biopsy involves removing small kidney tissue sample with needle under ultrasound guidance. Pathologists examine tissue under microscope, often using special staining and electron microscopy.
Genetic Counseling:
Genetic testing should be accompanied by genetic counseling, helping families understand results and their implications for health management and family planning.
Genetic Counseling Provides:
- Explanation of inheritance patterns and recurrence risks
- Discussion of testing options and limitations
- Help interpreting test results, including variants of uncertain significance
- Emotional support for dealing with genetic diagnosis
- Information about family testing and cascade screening
- Reproductive options for those with hereditary conditions
- Connection to support groups and resources
Frequently Asked Questions

What type of kidney diseases are hereditary?
Many kidney diseases have hereditary components, including polycystic kidney disease (the most common), Alport syndrome, Fabry disease, and various rare kidney conditions. These diseases result from genetic mutations passed from parents to children through different inheritance patterns.
Does kidney disease run in families?
Yes, kidney disease frequently runs in families due to shared genetic factors. Having a close relative with kidney disease increases your risk, though this doesn’t guarantee you’ll develop the condition. Environmental factors and lifestyle choices also play important roles.
What is the most common genetic disorder of the kidney?
Autosomal dominant polycystic kidney disease (ADPKD) represents the most common genetic kidney disorder, affecting approximately 1 in 500 to 1,000 people worldwide. It causes fluid-filled cysts to develop in the kidneys, gradually reducing kidney function over time.
How to test for genetic kidney disease?
Testing begins with blood and urine tests to assess kidney function. Imaging studies can reveal structural abnormalities, while genetic testing analyzes your DNA for specific mutations. A nephrologist can recommend appropriate tests based on your symptoms and family history.
What are the three early warning signs of kidney disease?
The three key early warning signs include changes in urination (frequency, color, or foaming), persistent fatigue despite adequate rest, and swelling in ankles, feet, or around the eyes. However, many people have no symptoms in early stages, making screening crucial for at-risk individuals.
Can stress cause kidney disease?
Stress alone doesn’t directly cause kidney disease, but chronic stress contributes to conditions like high blood pressure and diabetes that damage kidneys over time. Stress also affects lifestyle choices and medication adherence, indirectly impacting kidney health.
What is a rare genetic kidney disease?
Examples include Alport syndrome, Fabry disease, primary hyperoxaluria, and cystinosis. These conditions result from specific genetic mutations affecting kidney function but occur much less frequently than PKD. Despite their rarity, early diagnosis significantly improves outcomes.
Taking control of your kidney health
Understanding hereditary kidney disease represents the first step toward protecting your health and that of your family. Whether you’re managing a diagnosed condition or simply aware of family history, knowledge empowers better decisions about testing, treatment, and lifestyle modifications.
Key takeaways for managing hereditary kidney disease:
- Know your family history: Document kidney disease, diabetes, and hypertension across multiple generations
- Get tested appropriately: Request kidney function tests and genetic counseling if family history warrants
- Monitor regularly: Annual screening catches problems early when interventions are most effective
- Manage blood pressure: Maintaining healthy blood pressure protects kidney function regardless of underlying cause
- Adopt kidney-healthy lifestyle: Balanced diet, regular exercise, adequate hydration, and avoiding nephrotoxic substances
- Stay informed: New treatments emerge regularly for genetic kidney conditions
- Communicate with your doctor: Report any symptoms promptly and discuss concerns openly
- Consider genetic counseling: Understand inheritance patterns and implications for family planning
Patients who actively engage with their kidney health achieve better outcomes. Regular monitoring, adherence to treatment plans, and open communication with your healthcare team make all the difference in managing chronic kidney disease’s hereditary aspects.
Don’t wait for symptoms to appear—if kidney disease runs in your family, schedule a comprehensive evaluation with a qualified nephrologist. Early detection and intervention can preserve kidney function for decades, helping you maintain quality of life while researchers continue developing new treatments for genetic kidney disorders.