Are you concerned about the complications associated with immunosuppressive medications?
These potent drugs save lives but carry serious risks—infections, organ damage, and metabolic disorders threaten your health daily.
Understanding immunosuppressive medications side effects helps you manage treatment safely under expert guidance.
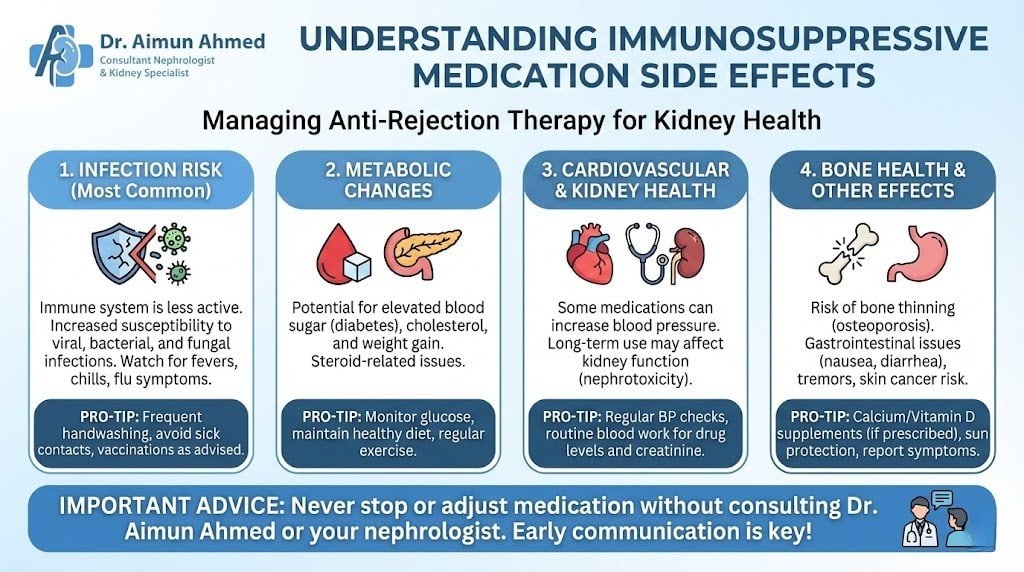
Immunosuppressive Medications Side Effects
When you receive medications that suppress your immune system, they serve a critical purpose—preventing organ rejection or controlling autoimmune diseases. However, these traditional pharmaceutical drugs affect your entire body, not just harmful immune activity.
Common adverse reactions include:
- Increased vulnerability to infections (bacterial, viral, fungal)
- High blood pressure requiring additional treatment
- Elevated blood sugar levels and diabetes development
- Kidney function complications
- Digestive issues including vomiting and nausea
- Tremors and neurological symptoms
- Bone density loss over time
- Increased cancer risk, particularly skin malignancies
Your healthcare professional monitors these effects carefully through regular blood tests, physical examinations, and screening programs. Each patient experiences different reactions based on medication type, dosage, and individual health factors.
Immunosuppressant Drugs List
Calcineurin Inhibitors:
- Tacrolimus (Prograf)
- Cyclosporine (Neoral, Sandimmune)
Antiproliferative Agents:
- Mycophenolate mofetil (CellCept)
- Mycophenolic acid (Myfortic)
- Azathioprine (Imuran)
mTOR Inhibitors:
- Sirolimus (Rapamune)
- Everolimus (Zortress)
Corticosteroids:
- Prednisone
- Methylprednisolone
Lymphocyte-Depleting Therapies:
- Tegoprubart (newer biological agent)
- Antithymocyte globulin (ATG)
Other Immunosuppressants:
- Belatacept (Nulojix)
- Methotrexate
- Cyclophosphamide
Your doctor selects specific combinations based on your transplanted organ, medical condition, and risk profile.
Immunosuppressive Drugs Side Effects
According to the Side Effects of Drugs Annuals—a comprehensive series of volumes surveyed in Meyler’s Side Effects of Drugs International Encyclopedia—these medications produce wide-ranging effects:
Neurological Effects:
- Headaches and migraines
- Tremors affecting hands and limbs
- Confusion or cognitive changes (rare)
- Sleep disturbances
Metabolic Complications:
- New-onset diabetes mellitus
- Weight gain or loss
- Cholesterol abnormalities
- Electrolyte imbalances
Dermatological Issues:
- Hair loss (often temporary)
- Acne and skin changes
- Increased photosensitivity
- Higher skin cancer risk
Gastrointestinal Problems:
- Nausea and vomiting
- Diarrhea or constipation
- Stomach ulcers
- Liver enzyme elevation
Cardiovascular Risks:
- High blood pressure
- Heart disease acceleration
- Fluid retention
Each medication carries unique risk profiles that your medical team considers when designing your treatment plan.
Side Effects of Stopping Immunosuppressive Drugs
Critical Warning: Never discontinue immunosuppressants without medical supervision.
Consequences of sudden discontinuation:
- Acute organ rejection (can occur within 24-72 hours)
- Severe autoimmune disease flares in non-transplant patients
- Irreversible organ damage from rejection episodes
- Potential graft loss requiring return to dialysis or re-transplantation
Proper discontinuation requires:
- Gradual dose reduction under doctor supervision
- Frequent monitoring of organ function
- Alternative therapy implementation when appropriate
- Clear communication with your healthcare team
If you experience intolerable side effects, talk with your doctor about adjusting medications rather than stopping them. Safer alternatives often exist.
What Is the Most Common Immunosuppressant Drug
Tacrolimus remains the most widely prescribed immunosuppressant globally for organ transplantation.
Why tacrolimus dominates:
- Superior efficacy in preventing acute rejection
- Well-established safety profile from decades of use
- Flexible dosing adjustments based on blood levels
- Compatibility with other immunosuppressive therapies
How tacrolimus works: It inhibits calcineurin, blocking pathways that activate T-cells in your immune response. This prevents your body from recognizing the transplanted organ as foreign tissue.
Monitoring requirements:
- Regular blood tests to maintain therapeutic levels
- Dose adjustments based on kidney function
- Careful attention to drug interactions
- Periodic assessment for long-term complications
Patients typically receive tacrolimus alongside other medications to create a balanced immunosuppression regimen while minimizing individual drug toxicity.
Immunosuppressant Drugs for Kidney Transplant Side Effects

Specific concerns for kidney transplant patients:
Nephrotoxicity (kidney damage from medications):
- Calcineurin inhibitors can harm the transplanted kidney
- Requires balancing rejection prevention against drug toxicity
- Regular creatinine and GFR monitoring essential
Cardiovascular complications:
- High blood pressure develops in 60-80% of patients
- Requires anti-hypertensive medications
- Increases long-term heart disease risk
Metabolic disturbances:
- Post-transplant diabetes affects 20-30% of recipients
- Weight management becomes challenging
- Cholesterol elevation common
Infection risks:
- Urinary tract infections more frequent
- Opportunistic infections require prophylactic antibiotics
- Viral reactivation (CMV, BK virus) threatens graft function
Bone health:
- Steroid-induced osteoporosis
- Increased fracture risk
- May require calcium, vitamin D, and bisphosphonates
Your nephrologist monitors these complications through comprehensive follow-up protocols, adjusting therapy to protect both your life and your transplanted kidney.
Long-Term Effects of Immunosuppressants
Years of continuous immunosuppression bring progressive risks:
Malignancy (Cancer):
- Skin cancer risk increases 10-fold
- Lymphomas more common than in general population
- Post-transplant lymphoproliferative disorder (PTLD)
- Requires annual dermatological screening and sun protection
Chronic infections:
- Recurrent bacterial infections
- Persistent viral infections (HPV, EBV)
- Fungal colonization
Organ dysfunction:
- Progressive kidney damage from medication toxicity
- Cardiovascular disease acceleration
- Liver complications in some patients
Musculoskeletal problems:
- Osteoporosis and fractures
- Avascular necrosis (bone death)
- Muscle weakness
Quality of life impacts:
- Cosmetic changes (weight gain, facial changes)
- Fatigue and reduced stamina
- Psychological stress from medication burden
Risk mitigation strategies:
- Regular cancer screening
- Vaccination programs (where safe)
- Lifestyle modifications
- Minimization protocols reducing drug exposure over time
Despite these risks, modern immunosuppression allows most transplant patients to enjoy decades of good health and quality of life.
Kidney Transplant Medications List
Standard triple-therapy regimen:
- Calcineurin inhibitor (tacrolimus or cyclosporine) – Backbone of therapy
- Antiproliferative agent (mycophenolate or azathioprine) – Prevents cell multiplication
- Corticosteroid (prednisone) – Reduces inflammation, often tapered to low doses
Additional medications commonly prescribed:
Prophylactic antibiotics:
- Trimethoprim-sulfamethoxazole (prevents pneumocystis)
- Valganciclovir (prevents CMV infection)
Supportive therapies:
- Antihypertensive drugs
- Cholesterol-lowering agents
- Diabetes medications if needed
- Proton pump inhibitors for stomach protection
Supplements:
- Calcium and vitamin D for bone health
- Iron if anemia develops
- Magnesium replacement
Alternative regimens for specific situations:
- Belatacept for patients with kidney toxicity
- mTOR inhibitors for cancer concerns
- Steroid-free protocols in selected patients
Each medication requires careful timing, specific instructions for taking with or without food, and awareness of potential interactions.
Tacrolimus Interactions with Antibiotics
Critical drug interactions occur through the cytochrome P450 3A4 enzyme system:
Antibiotics that INCREASE tacrolimus levels (risk of toxicity):
- Clarithromycin
- Erythromycin
- Azithromycin (mild effect)
- Fluoroquinolones (ciprofloxacin, levofloxacin)
Antibiotics that DECREASE tacrolimus levels (rejection risk):
- Rifampin (dramatic reduction)
- Rifabutin
Management strategies:
- Inform all healthcare professionals about your tacrolimus use
- Monitor blood levels more frequently during antibiotic treatment
- Adjust tacrolimus dosing temporarily under medical guidance
- Choose alternative antibiotics when possible
- Never take antibiotics without consulting your transplant team
Other significant interactions:
- Antifungal medications (fluconazole, itraconazole)
- Calcium channel blockers (diltiazem, verapamil)
- Grapefruit juice (avoid completely)
- St. John’s Wort and herbal supplements
- NSAIDs like ibuprofen (Voltaren)
Even over-the-counter medicines and supplements can affect tacrolimus levels. Always check with your healthcare provider before starting any new medication or supplement.
Tacrolimus Side Effects
Immediate side effects (within weeks to months):
- Tremors: Affecting hands, common especially at higher doses
- Headaches: Often improve as body adjusts
- Nausea and vomiting: Taking with food may help
- Diarrhea: Usually manageable with dietary changes
- Insomnia: May require timing adjustment of doses
Intermediate effects (months to years):
- New-onset diabetes: Requires blood sugar monitoring
- High blood pressure: Needs additional medication
- Kidney dysfunction: Paradoxical nephrotoxicity
- Electrolyte imbalances: Particularly high potassium, low magnesium
Long-term complications (years):
- Neurotoxicity: Rare but serious neurological effects
- Increased infection susceptibility: Ongoing vigilance required
- Hair changes: Thinning or texture changes
- Cosmetic effects: Facial changes, gum growth (less than cyclosporine)
When to contact your doctor immediately:
- Fever or signs of infection
- Severe tremors affecting function
- Confusion or personality changes
- Significant changes in urine output
- Persistent vomiting or diarrhea
Regular monitoring through blood tests helps maintain levels in the therapeutic range, minimizing both toxicity and rejection risk.
Kidney Immunosuppressant Uses
Beyond transplantation, these medications treat various kidney conditions:
Autoimmune kidney diseases:
- Lupus nephritis
- ANCA-associated vasculitis
- Membranous nephropathy
- Minimal change disease
Glomerular disorders:
- Focal segmental glomerulosclerosis (FSGS)
- IgA nephropathy (selected cases)
- Membranoproliferative glomerulonephritis
Systemic conditions affecting kidneys:
- Rheumatoid arthritis with kidney involvement
- Severe psoriasis
- Inflammatory bowel disease
Treatment principles remain consistent:
- Balance disease control against medication risks
- Use lowest effective doses
- Monitor kidney function carefully
- Adjust therapy based on response
- Consider steroid-sparing approaches when possible
For non-transplant kidney diseases, doctors often use different combinations than transplant protocols, sometimes including medications like methotrexate or cyclophosphamide for severe autoimmune conditions.
Immunosuppressants Examples
Classified by mechanism of action:
Calcineurin pathway blocking:
- Tacrolimus
- Cyclosporine
- Voclosporin (newer agent for lupus)
Cell proliferation inhibition:
- Mycophenolate
- Azathioprine
- Methotrexate
mTOR pathway blocking:
- Sirolimus
- Everolimus
Lymphocyte depleting:
- Tegoprubart
- Antithymocyte globulin
- Alemtuzumab
Anti-inflammatory steroids:
- Prednisone (systemic)
- Hydrocortisone
- Topical corticosteroids (for skin conditions)
Biological targeted therapies:
- Rituximab (anti-CD20)
- Belatacept (costimulation blockade)
- Eculizumab (complement inhibition)
Traditional disease-modifying agents:
- Cyclophosphamide
- Chlorambucil
- Leflunomide
Each medication class targets different immune pathways, allowing doctors to create customized treatment combinations that maximize effectiveness while minimizing individual drug toxicity. The goal is adequate immunosuppression without excessive complications.
Frequently Asked Questions
What is the most common side effect of immunosuppressive medications?
Increased susceptibility to infections represents the most universal complication of immunosuppression. Your weakened immune system struggles to fight bacteria, viruses, and fungi that healthy immune systems handle routinely.
This manifests as:
- More frequent common colds and flu
- Urinary tract infections
- Skin infections
- Opportunistic infections (CMV, pneumocystis, fungal)
- Slower healing of wounds
Prevention strategies include:
- Meticulous hand hygiene
- Avoiding sick contacts
- Prophylactic antibiotics for high-risk infections
- Prompt attention to fever or infection signs
- Staying current with recommended vaccinations (avoiding live vaccines)
Despite this risk, most patients learn to manage their increased infection susceptibility through vigilance and preventive measures.
What are 5 common side effects of medications?
The five most frequent complications across immunosuppressive therapies:
- Infections: As discussed above, increased vulnerability to all infection types
- High blood pressure: Develops in 60-80% of transplant patients, requiring antihypertensive treatment
- Elevated blood sugar/diabetes: Affects 20-30% of patients, particularly with tacrolimus and steroids
- Kidney problems: Even immunosuppressants given to protect kidneys can damage them over time
- Gastrointestinal disturbances: Nausea, vomiting, diarrhea, and stomach upset affect many patients
Additional common effects include:
- Tremors (especially with tacrolimus)
- Bone density loss
- Increased cancer risk
- Cosmetic changes
These effects require comprehensive monitoring programs and often necessitate additional medications or lifestyle interventions to manage safely.
What are the dangers of immunosuppressants?
Serious risks requiring ongoing medical supervision:
Life-threatening infections:
- Sepsis from bacterial infections
- Pneumocystis pneumonia (can be fatal)
- Cytomegalovirus disease affecting multiple organs
- Fungal infections like aspergillosis
Malignancy:
- Skin cancers (basal cell, squamous cell, melanoma)
- Post-transplant lymphoproliferative disorder
- Increased risk of common cancers
Organ damage:
- Progressive kidney dysfunction from nephrotoxic drugs
- Cardiovascular disease and heart attacks
- Liver toxicity with certain medications
Metabolic complications:
- Uncontrolled diabetes leading to complications
- Severe osteoporosis and fractures
- Hyperlipidemia accelerating atherosclerosis
However, important perspective:
For transplant patients, these risks are typically considered acceptable compared to:
- Losing the transplanted organ
- Returning to dialysis
- Reduced quality of life without transplant
For autoimmune disease patients, the risks balance against:
- Progressive organ damage from uncontrolled disease
- Severe disability from arthritis or other conditions
- Potential kidney failure from lupus or vasculitis
The key is careful monitoring, risk reduction strategies, and maintaining the lowest effective medication doses under expert supervision.
How do immunosuppressant drugs affect the body?
Comprehensive effects across body systems:
Immune system:
- Suppress T-cell activation and proliferation
- Reduce antibody production
- Decrease inflammatory cytokine release
- Impair immune memory responses
- Lower white blood cell counts
Kidneys:
- Calcineurin inhibitors cause vasoconstriction, reducing blood flow
- Direct tubular toxicity with some medications
- Electrolyte imbalances (high potassium, low magnesium)
- Potential for progressive fibrosis
Cardiovascular system:
- Increase blood pressure through multiple mechanisms
- Accelerate atherosclerosis development
- Cause fluid retention
- Alter lipid metabolism
Metabolic effects:
- Reduce insulin sensitivity and secretion
- Increase blood sugar levels
- Alter fat distribution and metabolism
- Affect bone formation and breakdown
Nervous system:
- Block calcineurin in neural tissue
- Can cause tremors and headaches
- Rarely cause more serious neurological effects
- May affect mood and cognition
Digestive system:
- Direct irritation of stomach lining
- Alter gut bacteria populations
- Affect nutrient absorption
- Cause nausea through central mechanisms
Cellular level:
- Inhibit specific enzyme pathways (calcineurin, mTOR)
- Block DNA synthesis in dividing cells
- Interfere with cell signaling
- Reduce protein production
This system-wide impact explains why immunosuppressants require comprehensive medical management. Your body adapts to these medications over time, but ongoing monitoring remains essential to balance therapeutic benefits against potential complications. Regular follow-up with your healthcare team ensures early detection and management of adverse effects while maintaining adequate immunosuppression to protect your transplant or control your autoimmune condition.
Expert Care for Immunosuppression Management
Prof. Aimun Ahmed | Consultant Nephrologist & Kidney Specialist
With over three decades of specialized experience and more than 5,000 patients managed, Prof. Aimun Ahmed delivers world-class kidney care grounded in safety and precision. Based at Lancashire Teaching Hospitals (UK), he specializes in:
- Chronic Kidney Disease (CKD) management
- Transplant Medicine and immunosuppression optimization
- Hypertension control in kidney patients
- Complex autoimmune kidney disorders
Prof. Ahmed offers evidence-based, compassionate care to patients globally, ensuring clear communication about medication risks and benefits, personalized treatment outcomes, and comprehensive monitoring protocols. His approach prioritizes patient safety while maximizing treatment effectiveness, helping you navigate the complexities of immunosuppressive therapy with confidence.
For expert guidance on managing immunosuppressive medications and their side effects, Prof. Ahmed provides the specialized knowledge and experience necessary to optimize your treatment while minimizing complications.