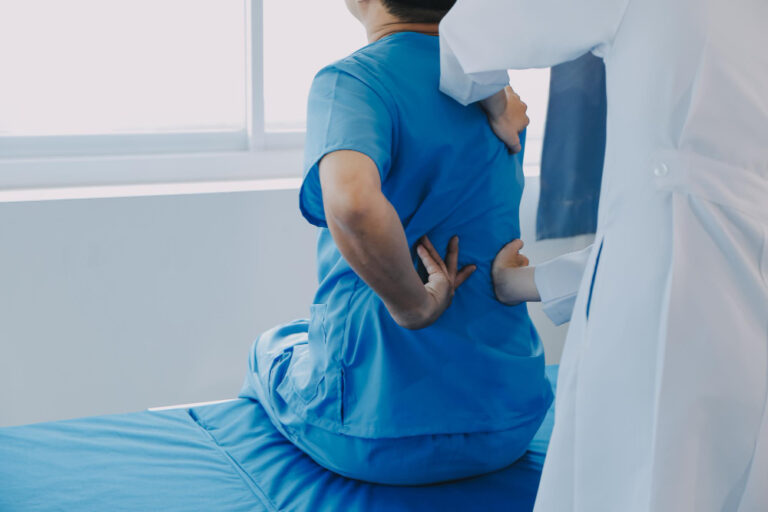
Your kidneys filter waste from your blood every single day, but what happens when they suddenly stop working?
Thousands of people experience a rapid decline in kidney function each year, often without warning, leading to serious complications that can affect every organ in your body.
Understanding acute kidney injury can help you recognize the signs early and seek treatment before permanent damage occurs.
Acute kidney injury represents one of the most common complications seen in hospitals worldwide. Unlike chronic kidney disease, which develops slowly over years, AKI happens quickly—sometimes within hours or days. Your kidneys lose their ability to filter waste products from your blood, causing dangerous buildups of toxins and fluid imbalances that can affect your heart, lungs, and brain.
The good news? With prompt recognition and proper treatment, many people recover full kidney function. This guide walks you through everything you need to know about acute kidney injury, from the earliest warning signs to the latest treatment approaches used by specialists like Prof. Aimun Ahmed at Lancashire Teaching Hospitals.

What Is Acute Kidney Injury?
Acute kidney injury happens when your kidneys suddenly lose their filtering ability. This rapid decline in renal function is characterized by the accumulation of waste products and fluid imbalances that develop over hours or days. Your glomerular filtration rate—the measurement of how efficiently your kidneys clean blood—drops significantly.
When doctors talk about acute kidney injury, they’re describing a condition where nitrogenous products like creatinine and urea build up in your bloodstream. Your kidneys can’t maintain the delicate electrolyte balance your body needs, and fluid regulation becomes disrupted. This creates complications that can affect every organ system.
Acute kidney injury ranges from mild cases where function dips slightly to severe situations requiring dialysis. The KDIGO guideline helps medical professionals stage the severity and guide the treatment of AKI appropriately.
Acute Kidney Injury Causes
Several factors can trigger an episode of kidney failure. Understanding these causes helps you recognize your risk and take preventive steps.
- Reduced blood flow to your kidneys tops the list. Severe dehydration, major blood loss, heart failure, or extremely low blood pressure can all decrease the blood supply your kidneys need to function. This prerenal type of injury affects the kidneys before blood even reaches them.
- Direct kidney damage happens when infections, toxic medications, or autoimmune diseases harm the kidney tissue itself. Certain antibiotics, pain relievers, and imaging dyes can damage the intrinsic kidney structures when used for prolonged periods or in high doses.
- Blocked urine flow creates postrenal injury. Kidney stones, tumors, or an enlarged prostate can prevent urine from leaving your body, causing pressure to build up and decrease kidney function.
Recent data shows that COVID-19 can lead to acute kidney injury in hospitalized patients. Surgery, particularly cardiac procedures, also poses significant risk. Critically ill people in hospital settings develop AKI more frequently due to the combination of severe illness and multiple medications.
Acute Kidney Injury Symptoms
Identifying the signs early is vital. Because AKI affects how you handle fluids and waste, the symptoms are often physical and noticeable. You might notice you aren’t passing urine as often as usual, or the amount is very small.
Other common symptoms include:
- Swelling (edema) in your legs, ankles, or around your eyes due to fluid accumulation.
- Fatigue and confusion caused by the buildup of waste products in the blood.
- Shortness of breath if fluid builds up in the lungs.
- Nausea or chest pain/pressure.
It is worth noting that some patients show no obvious signs, and the condition is only spotted through lab tests seeing a rise in creatinine levels.
Acute Kidney Injury Stages
Medical professionals use the KDIGO staging system to classify how severe your condition has become:
- Stage 1: represents mild injury. Your creatinine levels increase slightly, or urine output decreases to less than 0.5 mL/kg/hour for six to twelve hours. Many patients at this stage recover with proper management.
- Stage 2: indicates moderate injury. Creatinine levels double from baseline, or urine output stays low for twelve hours or more. This stage requires closer monitoring and more intensive treatment.
- Stage 3: signals severe kidney injury. Creatinine triples, urine output remains minimal for twenty-four hours, or you need dialysis. This stage carries increased mortality risk and potential for progression to chronic kidney disease.
Understanding these stages helps your healthcare team determine the appropriate treatment approach and predict outcomes. Prof. Ahmed’s three decades of clinical experience have shown that catching AKI in stage 1 provides the best chance for complete recovery.
Diagnosing the Condition
When you visit a specialist like Prof. Aimun Ahmed, the diagnosis process is thorough. It starts with a clinical assessment of your history. Have you recently had surgery? Are you taking new medications?
Key Diagnostic Tests:
- Urine Output Measurements: Tracking how much you urinate over 24 hours.
- Blood Tests: Checking levels of urea nitrogen and creatinine to estimate the glomerular filtration rate (GFR).
- Imaging: Ultrasounds or CT scans to look for blockages or physical abnormalities in the kidneys.
- Kidney Biopsy: In rare cases, a small tissue sample is taken to find intrinsic causes of damage.
Acute Kidney Injury Treatment

The treatment of AKI largely depends on what caused it in the first place. The goal is to restore renal function and prevent waste accumulation while the kidneys heal themselves.
- Managing Fluids: If you are dehydrated, you will receive IV fluids. Conversely, if you are retaining too much fluid, diuretics (water pills) may be prescribed to help expel it.
- Balancing Electrolytes: High levels of potassium or acid in the blood can be dangerous for your heart. Medications are used to normalize these levels.
- Medication Review: stopping drugs that might be worsening the damage.
- Dialysis: In severe cases where the kidneys essentially shut down, short-term dialysis may be needed to take over the filtration job until the kidneys recover.
Acute Kidney Injury Recovery Time
Recovery from an episode of acute renal failure varies significantly between patients.
Mild cases often resolve within a few days to a week with proper treatment. Your kidney function returns to normal, and you can resume regular activities without restrictions.
Moderate injury might require several weeks of recovery. During this period, your kidneys gradually regain their filtering ability. You’ll need regular blood tests to monitor progress and dietary adjustments to support healing.
Severe AKI can take months to resolve. Some patients recover most of their kidney function but don’t quite return to baseline. Others develop chronic kidney disease after a severe episode.
Several factors influence recovery time: your age, overall health, the cause of injury, how quickly treatment began, and whether you had existing kidney disease. People who receive prompt, evidence-based care from experienced nephrologists like Prof. Ahmed have the best outcomes.
Acute Kidney Injury ICD-10
Healthcare providers use the ICD-10 coding system to classify medical conditions for diagnosis, billing, and research purposes.
The primary code for acute kidney injury is N17. This breaks down into more specific codes:
- N17.0: Acute kidney failure with tubular necrosis
- N17.1: Acute kidney failure with acute cortical necrosis
- N17.2: Acute kidney failure with medullary necrosis
- N17.8: Other acute kidney failure
- N17.9: Acute kidney failure, unspecified
These codes help track AKI data across hospitals and contribute to research studies that improve understanding and treatment. They also ensure proper documentation of your condition in medical records.
Complications and Risks
If left untreated, AKI can lead to serious, life-threatening complications. The most immediate risk is hyperkalemia (high potassium), which can cause muscle weakness and dangerous heart arrhythmias.
Fluid buildup in the lungs can cause respiratory failure. Furthermore, the condition can lead to permanent kidney damage (End-Stage Renal Disease), requiring permanent dialysis or a transplant. There is also a correlation with increased mortality in hospital settings if the AKI is severe and not managed aggressively.
Prevention Strategies
Can you prevent AKI? In many cases, yes.
- Stay Hydrated: Drinking enough water helps flush out kidneys, especially during exercise or hot weather.
- Be Careful with Meds: Long-term use of NSAIDs (like ibuprofen) can damage kidneys. Always follow the label.
- Manage Chronic Conditions: Keeping diabetes and high blood pressure under control reduces the strain on your kidneys.
- Review Risks in Hospital: If you are getting contrast dye for a scan, ask about the risks to your kidneys.
The Role of Specialized Care
Navigating kidney health can be complex. This is where the expertise of Prof. Aimun Ahmed becomes invaluable. With over three decades of experience and more than 5,000 patients managed, Dr. Ahmed doesn’t just treat the numbers on a chart; he treats the person.
Based at Lancashire Teaching Hospitals (UK), Prof. Ahmed specializes in handling the delicate transition from acute renal failure to recovery, ensuring that a temporary injury doesn’t become a lifelong burden. His approach combines evidence-based medicine with compassionate, clear communication, ensuring you understand every step of your journey.
Frequently Asked Questions
What is an acute kidney injury?
Acute kidney injury is a sudden decline in kidney function that happens over hours or days. Your kidneys lose their ability to filter waste products and excess fluid from your blood, leading to dangerous buildups of toxins and electrolyte imbalances. Unlike chronic kidney disease that develops slowly, AKI strikes quickly and requires immediate medical attention.
What is the most common cause of acute kidney injury?
The most common cause of acute kidney injury is reduced blood flow to the kidneys, known as prerenal AKI. This can result from severe dehydration, major blood loss, heart failure, or extremely low blood pressure. In hospital settings, surgery and medications are also frequent triggers for kidney injury.
How to fix acute kidney injury?
Fixing acute kidney injury depends on the underlying cause. Treatment might involve IV fluids to restore blood flow, stopping harmful medications, removing blockages in the urinary tract, or using dialysis for severe cases. The key is identifying the cause quickly and starting appropriate treatment. Many patients recover full kidney function with prompt medical care.
What are the three stages of acute kidney injury?
The three stages are classified by how high the creatinine levels rise:
- Stage 1: Slight rise in creatinine or lower urine output.
- Stage 2: Moderate rise in creatinine.
- Stage 3: Severe rise in creatinine, often requiring dialysis.
Conclusion
Acute kidney injury is a serious condition, but it is not a hopeless one. With rapid diagnosis and the right management, the kidneys often heal. Whether you are dealing with a sudden decline in function or worried about potential risks, knowledge is your best defense. If you suspect you are at risk or are experiencing symptoms, seeking expert clinical advice immediately is the best step you can take for your long-term health.