When your kidneys start losing their ability to filter blood properly, the changes don’t happen overnight. The condition develops slowly, often silently, giving you little warning until significant damage has occurred. This progressive decline in kidney function affects millions worldwide, yet many people remain unaware they have it until reaching advanced stages.
Living with chronic kidney disease means understanding how your body processes waste, maintains fluid balance, and regulates essential functions that keep you alive. Your kidneys work tirelessly, filtering roughly 200 liters of blood daily, removing toxins, and producing hormones that control blood pressure and red blood cell production. When these vital organs begin failing, every system in your body feels the impact.
The good news? Early detection changes everything. With proper management, you can slow progression, prevent complications, and maintain quality of life for years. This guide provides comprehensive information grounded in three decades of clinical practice and thousands of patient outcomes, helping you understand the basics of chronic kidney disease and make informed decisions about your health.

What Is Chronic Kidney Disease?
Chronic kidney disease represents a type of long-term kidney disease where your kidneys gradually lose their ability to filter blood effectively. Unlike acute kidney problems that develop suddenly and may resolve quickly, CKD involves the sustained presence of abnormal kidney function lasting three months or longer.
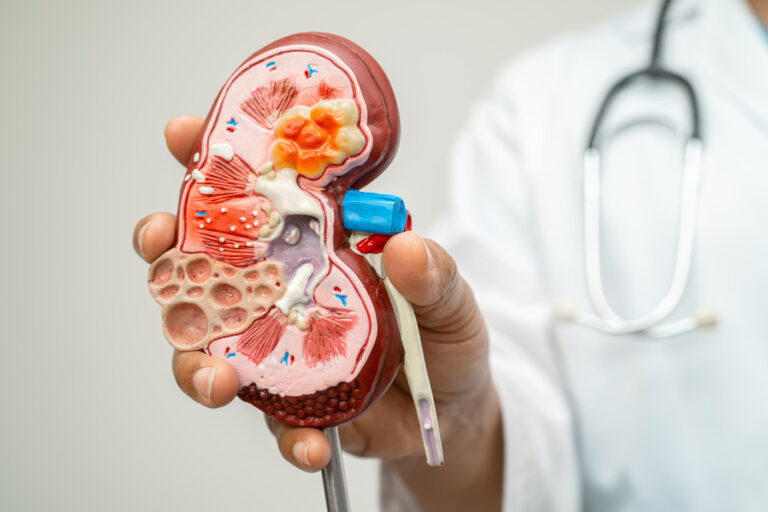
Think of your kidneys as sophisticated filtration systems. Each kidney contains about one million tiny filtering units called nephrons. These structures clean your blood by removing waste products and excess fluid while keeping essential substances like proteins and red blood cells where they belong. When CKD develops, these nephrons become damaged and can’t perform their duties properly.
The condition progresses through five distinct stages based on how well your kidneys filter blood. Doctors measure this using a calculation called eGFR (estimated glomerular filtration rate). This number tells them what percentage of normal kidney function remains. In early stages, you might retain 60-89% of normal function with minimal symptoms. By later stages, function drops below 15%, approaching kidney failure.
Prof. Aimun Ahmed emphasizes that CKD is remarkably common yet frequently overlooked. Approximately one in seven adults lives with some degree of kidney disease, though many remain unaware. The gradual nature of progression means damage accumulates slowly over time, making early detection through routine screening essential for preserving kidney health.
Chronic Kidney Disease Causes
Understanding what drives this type of long-term kidney disease is the first step in prevention. CKD doesn’t usually happen overnight; it is often the result of other underlying health issues that stress the kidneys over years.
The two most common causes are diabetes and high blood pressure.
- Diabetes: When blood sugar remains high, it damages the tiny filtering units in the kidneys. Over time, this stress leads to renal damage and eventually failure.
- High Blood Pressure: Uncontrolled pressure forces blood against the vessel walls in your kidneys. This weakens them, reducing their ability to filter wastes.
Other factors include genetic disorders like polycystic kidney disease, prolonged obstruction of the urinary tract (from kidney stones or enlarged prostate), and recurrent kidney infections. It is also important to note that the sustained presence of abnormal kidney function can be triggered by the long-term use of certain medications, such as NSAIDs, which can lead to toxicity.
Dr. Aimun Ahmed emphasizes that identifying these root causes early is crucial. If you manage the cause—like keeping your sugar in control—you can significantly slow the progression of the disease.
Chronic Kidney Disease Symptoms
One of the most challenging aspects of CKD is its subtle nature during early stages. Many people with mild to moderate kidney disease feel completely normal and only discover their condition through routine blood or urine tests. As function declines, however, symptoms gradually emerge.
Early warning signs often go unnoticed because they’re vague and easily attributed to other causes. You might experience:
- Fatigue and decreased energy that doesn’t improve with rest
- Difficulty concentrating or mental fog
- Sleep problems, including trouble falling asleep or staying asleep
- Dry, itchy skin that doesn’t respond well to moisturizers
- Increased need to urinate, especially at night
Advanced symptoms become more apparent as kidney function deteriorates further. These include:
- Swelling in feet, ankles, legs, or hands from fluid retention
- Puffiness around the eyes, particularly in the morning
- Persistent foaming or bubbling in urine, indicating protein loss
- Blood in urine, making it appear pink, red, or cola-colored
- Decreased urine output despite drinking normal amounts of fluid
Systemic effects develop when kidneys can no longer maintain proper body chemistry. Patients may experience:
- Nausea and vomiting, especially in the morning
- Loss of appetite and unintended weight loss
- Muscle cramps and twitching
- Shortness of breath from fluid buildup in lungs
- Chest pain if fluid accumulates around the heart
As waste products accumulate in blood, they affect multiple body systems. Anemia develops because damaged kidneys produce less erythropoietin, the hormone stimulating red blood cell production. This contributes to fatigue and weakness. Bone disease occurs when kidneys fail to activate vitamin D properly, leading to calcium imbalances that weaken bones.
Prof. Ahmed stresses that symptom severity doesn’t always correlate with kidney function levels. Some patients with significantly reduced function feel relatively well, while others with moderate disease experience troublesome symptoms. This variability underscores why regular monitoring through blood and urine tests proves more reliable than symptoms alone for tracking disease progression.
Chronic Kidney Disease Stages

Medical professionals classify this condition into five distinct stages based on eGFR measurements and the presence of kidney damage. Understanding your stage helps determine treatment intensity and what to expect moving forward.
- Stage 1 involves normal or high kidney function (eGFR ≥90) but with evidence of damage, such as protein in urine. At this point, lifestyle modifications and treating underlying conditions can prevent progression. Many people feel completely normal during this stage.
- Stage 2 shows mild reduction in function (eGFR 60-89) with signs of damage. Symptoms remain minimal, but this stage requires close monitoring and aggressive management of risk factors. Blood pressure control becomes paramount.
- Stage 3 divides into 3a (eGFR 45-59) and 3b (eGFR 30-44), representing moderate decline. Waste products begin accumulating in blood, potentially causing fatigue, swelling, and changes in urination patterns. Dietary modifications and medication adjustments become necessary.
- Stage 4 indicates severe reduction (eGFR 15-29), requiring preparation for renal replacement therapy. Complications including anemia, bone disease, and electrolyte imbalances need active management. Quality of life significantly impacts daily activities.
- Stage 5, also called end-stage kidney disease (ESKD) or kidney failure, means function has dropped below 15. At this point, dialysis or transplantation becomes necessary for survival as kidneys can no longer remove enough waste and fluid to sustain life.
Each stage progression isn’t inevitable. With appropriate interventions, many patients stabilize at stage 3 for years, avoiding the need for dialysis. Regular monitoring through blood tests and urine analysis helps track progression and adjust treatment plans accordingly.
Risk Factors for Kidney Disease
Certain conditions and characteristics increase your likelihood of developing CKD. Recognizing these risk factors enables earlier screening and more aggressive prevention efforts.
- Diabetes and high blood pressure top the list as the most significant risk factors. If you have either condition, your risk increases substantially. Having both multiplies risk even further. Maintaining good control of blood sugar and blood pressure dramatically reduces your chances of developing kidney problems.
- Cardiovascular disease shares common risk factors with kidney disease. Heart disease, previous heart attack, or stroke indicate higher kidney disease risk. The connection runs both directions—kidney disease also increases cardiovascular risk, creating interconnected health challenges.
- Family history plays an important role. If close relatives have kidney disease, your risk increases, partly due to shared genetic factors and partly from similar lifestyle and environmental exposures. Certain inherited conditions like polycystic kidney disease directly cause CKD.
- Age represents a non-modifiable risk factor. Kidney function naturally declines with age, and CKD becomes more common after 60. However, this doesn’t mean kidney disease is inevitable—many older adults maintain healthy kidney function throughout their lives.
- Obesity strains kidneys and contributes to diabetes and high blood pressure, compounding risk. Maintaining a healthy weight protects kidney function and reduces overall disease risk.
- Smoking damages blood vessels throughout your body, including those in kidneys. It accelerates kidney disease progression and interferes with medications used to manage the condition. Quitting smoking is one of the most impactful actions you can take for kidney health.
- Other factors that elevate risk include:
- African, Asian, or Hispanic ancestry, which increases genetic susceptibility
- Prolonged use of medications like NSAIDs (ibuprofen, naproxen) that can damage kidneys
- Recurring urinary tract infections or kidney infections
- Autoimmune diseases affecting multiple organs
- Previous acute kidney injury episodes
Prof. Ahmed recommends that anyone with multiple risk factors undergo regular screening through simple blood and urine tests. Early detection combined with lifestyle modifications can prevent or significantly delay kidney disease development.
Diagnosis and Testing for Kidney Disease
Detecting kidney disease early requires specific tests that measure kidney function and identify damage. Many cases are discovered during routine health screenings rather than from symptoms.
Blood tests
Blood tests provide the most direct assessment of kidney function. The serum creatinine test measures this waste product that healthy kidneys normally filter out. When kidneys struggle, creatinine accumulates in blood. Doctors use your creatinine level, along with age, sex, and body size, to calculate eGFR—the key indicator of kidney function.
The blood urea nitrogen (BUN) test measures another waste product. While less precise than creatinine for kidney function, elevated BUN combined with high creatinine strengthens the diagnosis. Additional blood tests check electrolyte levels, including potassium and phosphorus, which kidneys help regulate.
Urine tests
Urine tests detect abnormalities that signal kidney damage even when blood tests appear normal. The urine albumin test measures whether protein is leaking into urine—a common early sign of kidney damage. Healthy kidneys retain protein in blood, so finding it in urine indicates filtering problems.
A complete urinalysis examines multiple urine characteristics, including the presence of blood cells, bacteria, or abnormal crystals. The albumin-to-creatinine ratio (ACR) provides a more accurate measure of protein loss than a simple dipstick test.
Imaging studies
Imaging studies visualize kidney structure. Ultrasound, the most common imaging method, reveals kidney size, shape, and the presence of cysts, stones, or tumors. It’s painless and uses no radiation. CT scans or MRIs provide more detailed images when needed to evaluate complex problems.
Kidney biopsy
Kidney biopsy involves removing a tiny tissue sample for microscopic examination. This procedure, performed under local anesthesia, helps diagnose the specific type of kidney disease when the cause remains unclear. The information gained guides treatment decisions, though biopsy isn’t necessary for all patients.
Prof. Ahmed emphasizes the importance of trending results over time rather than focusing on single test values. Kidney function naturally fluctuates slightly, and isolated abnormalities might not indicate disease. Repeated testing showing sustained abnormalities for three months or longer confirms a chronic condition.
Chronic Kidney Disease Treatments
When discussing treatment options, the primary goal is to stop the disease from getting worse. While there is no cure for chronic kidney disease, proper management can keep you living a full life for years.
- Medication: Doctors often prescribe drugs to control blood pressure (like ACE inhibitors) which also protect the kidneys. You may also need medication to lower cholesterol, treat anemia, or relieve swelling.
- Dialysis: If the disease progresses to failure, you may need dialysis. This process artificially removes waste and extra fluid from your blood. There are two main types: hemodialysis (using a machine) and peritoneal dialysis (using the lining of your belly to filter).
- Kidney Transplant: For many, this is the best option for later stages. It involves receiving a healthy kidney from a donor. Dr. Ahmed specializes in Transplant Medicine, ensuring patients understand the safety protocols and long-term care required for a successful transplant.
- Conservative Care: Some patients choose to manage symptoms without dialysis, focusing on quality of life and comfort.
Chronic Kidney Disease Diet
Your diet plays a massive role in slowing kidney damage. When your kidneys are compromised, they can’t filter certain nutrients as well as they used to. A “renal diet” is restrictive but necessary.
You generally need to limit:
- Sodium: Too much salt increases blood pressure and causes fluid buildup.
- Potassium: Damaged kidneys can’t filter potassium well. High levels can cause dangerous heart rhythms. Foods like bananas, oranges, and potatoes might need to be limited.
- Phosphorus: High phosphorus can pull calcium from your bones. You may need to limit dairy, nuts, and dark colas.
- Protein: While your body needs protein, eating too much creates extra waste that the kidneys must work hard to remove.
Dr. Ahmed’s team often works with dietitians to create personalized plans. Eating the right foods helps lower the workload on your kidneys and prevents the accumulation of metabolic wastes.
Preventing Chronic Kidney Disease
Prevention offers the best approach to kidney disease. Many cases can be avoided entirely through lifestyle choices and management of underlying health conditions.
- Control blood sugar if you have diabetes. Maintaining hemoglobin A1C below 7% significantly reduces kidney damage risk. This requires consistent monitoring, medication adherence, dietary management, and regular physical activity. Work closely with your healthcare provider to achieve optimal control.
- Manage blood pressure through lifestyle and medication when necessary. Target blood pressure for kidney protection typically aims for less than 130/80 mmHg, though your doctor may set different goals based on your circumstances. Home blood pressure monitoring helps track progress.
- Maintain a healthy weight through balanced nutrition and regular exercise. Obesity increases diabetes and high blood pressure risk while directly stressing kidneys. Even modest weight loss provides substantial benefits.
- Exercise regularly for at least 150 minutes weekly of moderate-intensity activity like brisk walking. Physical activity helps control weight, blood pressure, blood sugar, and cholesterol while boosting overall health.
- Quit smoking and limit alcohol. Smoking damages blood vessels throughout your body, including kidneys, and accelerates disease progression. Alcohol in excess can raise blood pressure and harm kidneys.
- Avoid medications that harm kidneys when possible. NSAIDs (ibuprofen, naproxen) can damage kidneys, especially with long-term use or high doses. Certain antibiotics, contrast dyes used in imaging tests, and herbal supplements may also cause problems. Always inform healthcare providers about your kidney function before starting new medications.
- Stay hydrated by drinking adequate water. Proper hydration helps kidneys flush toxins and prevents kidney stone formation. However, excessive water intake doesn’t improve kidney function and can be harmful in advanced disease.
- Get screened regularly if you have risk factors. Simple blood and urine tests detect problems early when interventions work best. Annual screening is recommended for those with diabetes, high blood pressure, cardiovascular disease, or family history of kidney disease.
Prof. Ahmed emphasizes that prevention and early intervention dramatically improve outcomes. Many patients who develop early-stage kidney disease can prevent progression through diligent management of risk factors and adherence to treatment recommendations.
Read: Guide to Understanding Kidney Transplant Rejection
Complications of Kidney Disease
CKD affects multiple body systems beyond the kidneys themselves. Understanding potential complications helps you recognize problems early and work with your healthcare team to prevent or manage them.
- Cardiovascular disease represents the most serious complication. People with kidney disease face markedly higher risk of heart attack, stroke, and heart failure. The connection runs both directions—kidney disease worsens heart disease, and heart disease accelerates kidney decline. Managing blood pressure, cholesterol, and diabetes becomes crucial for protecting both organs.
- Anemia develops because damaged kidneys produce insufficient erythropoietin, the hormone triggering red blood cell production. Low red blood cell counts cause fatigue, weakness, shortness of breath, and decreased ability to concentrate. Treatment includes iron supplementation and erythropoiesis-stimulating medications.
- Bone disease occurs when kidneys fail to activate vitamin D properly and can’t maintain proper calcium and phosphorus balance. This leads to weakened, brittle bones prone to fractures. High phosphorus levels also cause dangerous calcium deposits in blood vessels and soft tissues. Treatment includes vitamin D supplements, phosphate binders, and sometimes medications to regulate parathyroid hormone.
- Fluid retention happens when kidneys can’t remove excess water from blood. Fluid accumulates in tissues, causing swelling in feet, ankles, and legs. Severe fluid overload can lead to pulmonary edema—fluid in lungs causing severe shortness of breath—or fluid around the heart.
- Electrolyte imbalances pose serious risks. High potassium levels (hyperkalemia) can cause dangerous heart rhythm abnormalities. Acidosis develops when kidneys can’t eliminate acids produced by metabolism, making blood too acidic. These imbalances require dietary modifications and sometimes medications.
- Malnutrition affects many patients with advanced kidney disease. Loss of appetite, nausea, dietary restrictions, and increased protein losses lead to inadequate nutrition. Maintaining proper nutrition becomes challenging but remains essential for health and quality of life.
- Immune system impairment increases infection risk. Kidney disease and its treatments weaken immune defenses, making patients more susceptible to infections and slower to recover. Vaccinations become especially important.
- Cognitive decline and mental health issues occur more frequently in kidney disease patients. Depression and anxiety are common, partly from dealing with chronic illness and partly from biochemical changes affecting brain function.
Prof. Ahmed monitors patients regularly for these complications, implementing preventive strategies and treatments before problems become severe. He emphasizes that many complications can be prevented or minimized through proactive management and adherence to treatment recommendations.
Chronic Kidney Disease Alterations in Health
CKD is rarely just about the kidneys; it is a systemic condition. It triggers a domino effect throughout the body.
Because the kidneys produce hormones that regulate other bodily functions, loss of function leads to hormonal imbalances. You might experience a weakened immune system, making you more prone to infections. Your body’s balance of acid and base gets disrupted (metabolic acidosis), leading to muscle wasting and worsening bone health.
Furthermore, CKD affects your mental health. The stress of managing a chronic illness can lead to depression or anxiety. Dr. Ahmed believes in holistic care, addressing not just the physical damages but the overall well-being of the patient.
Chronic Kidney Disease and Low Hemoglobin
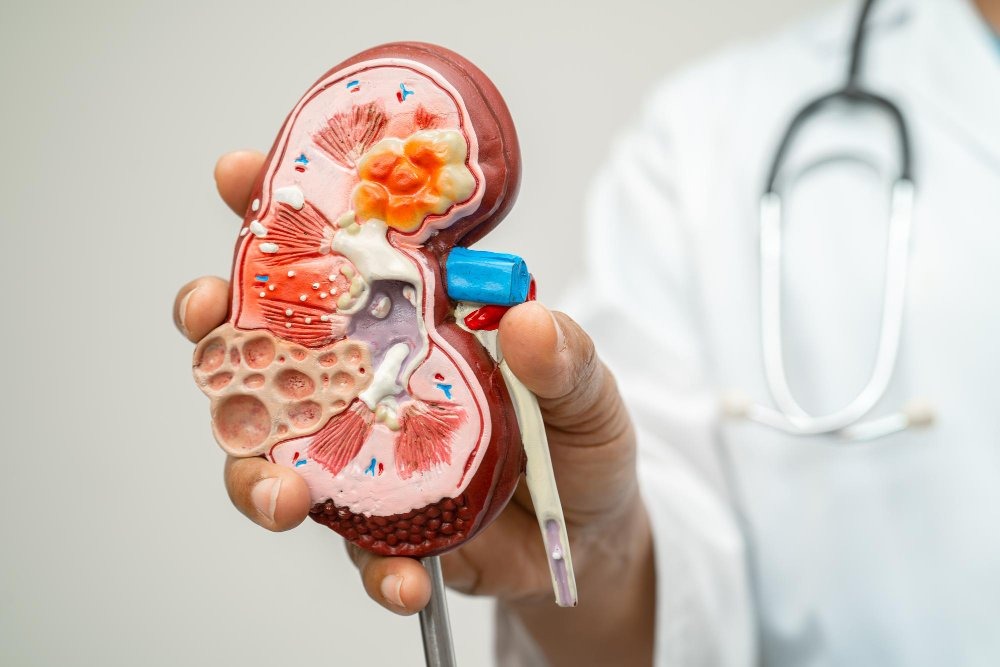
Anemia is a very common complication of CKD. Healthy kidneys produce a hormone called erythropoietin (EPO), which signals your bone marrow to make red blood cells.
When kidneys are damaged, they produce less EPO. This leads to a drop in red blood cells, meaning less oxygen is carried to your muscles and brain. This is why patients often feel cold, tired, and short of breath.
Treating this usually involves iron supplements or injections of synthetic EPO stimulating agents (ESAs) to help the body produce more blood cells. Restoring hemoglobin levels is vital for improving energy levels and cardiac health.
Chronic Kidney Disease and Heart Failure
The heart and kidneys are intimately connected. In fact, heart disease is the leading cause of death for people with CKD, not the kidney disease itself.
When kidneys fail to excrete salt and fluid, the volume of blood increases, forcing the heart to pump harder. This leads to high blood pressure and eventually heart failure. Conversely, a weak heart can’t pump enough blood to the kidneys, causing further renal damage.
Managing this connection is a core part of Dr. Ahmed’s practice. Controlling blood pressure and fluid intake protects both the heart and the kidneys simultaneously.
Chronic Kidney Disease and Leg Pain
Patients frequently complain of leg pain, which can stem from several CKD-related issues.
- Cramps: Electrolyte imbalances, specifically regarding calcium and phosphorus, often cause severe muscle cramps, especially at night.
- Neuropathy: High levels of toxins (uremia) in the blood can damage nerve endings, leading to a sensation of pins and needles or burning in the legs.
- Peripheral Artery Disease (PAD): CKD speeds up the hardening of arteries, reducing blood flow to the limbs. This can cause pain when walking.
If you experience persistent leg pain, it isn’t just “part of aging”—it’s a signal that your management plan might need adjustment.
Chronic Kidney Disease and Gastrointestinal Disorders
As waste products build up in the blood (uremia), the digestive system takes a hit. Nausea and vomiting are classic signs that the kidneys are struggling to clean the body.
You might also experience a metallic taste in your mouth or “uremic breath,” which smells like ammonia. Gastritis and peptic ulcers are also more prevalent in kidney patients. Loss of appetite is dangerous because it leads to malnutrition, weakening the body further. Managing these GI issues is essential to ensure the patient remains strong enough to undergo treatments like dialysis.
Chronic Kidney Disease Bone Mineral Disorder
Healthy kidneys convert Vitamin D into its active form, which the body needs to absorb calcium. They also keep phosphorus levels in check.
In CKD, this balance collapses. Phosphorus levels rise, and Vitamin D levels drop. To compensate, the body steals calcium from the bones to keep blood levels steady. This condition, known as CKD-Mineral and Bone Disorder (CKD-MBD), makes bones weak and brittle, increasing the risk of fractures.
Treatment involves taking phosphate binders with meals and Vitamin D supplements to protect bone integrity.
Chronic Kidney Disease Blood Test Results
Diagnosing and monitoring CKD relies heavily on tests. Understanding your report can help you have better conversations with Dr. Ahmed.
- Serum Creatinine: Creatinine is a waste product from muscle wear. Healthy kidneys remove it. High levels in the blood suggest kidney impairment.
- eGFR: Calculated using your creatinine level, age, and gender. This determines your stage.
- BUN (Blood Urea Nitrogen): Measures urea nitrogen, a breakdown product of protein. High levels indicate the kidneys aren’t filtering well.
- Albumin-to-Creatinine Ratio (ACR): A urine test that checks for albumin (a type of protein). Protein shouldn’t be in the urine; its presence is an early sign of damage.
Regular testing allows Dr. Ahmed to track the progressive nature of the disease and adjust options before complications become severe.
Frequently Asked Questions
What are 5 symptoms of chronic kidney disease?
Five common symptoms include persistent fatigue that doesn’t improve with rest, swelling in feet and ankles from fluid retention, changes in urination patterns (especially increased nighttime urination), difficulty concentrating or mental fog, and loss of appetite or nausea. However, many people with early-stage kidney disease experience no symptoms at all, making screening tests crucial for detection.
Can you live a long life with kidney disease?
Yes, many people live long, fulfilling lives with kidney disease. Early-stage disease often progresses slowly or remains stable with proper management. Even patients with advanced disease or kidney failure can live for decades with dialysis or transplant.
Outcomes depend on disease severity, underlying causes, how well treatments work, and adherence to medical recommendations. Managing diabetes, blood pressure, and cardiovascular risk factors significantly extends life expectancy.
What is stage 4 kidney disease?
Stage 4 represents severe reduction in kidney function, with eGFR between 15-29 milliliters per minute. At this stage, kidneys have lost 70-85% of normal function. Waste products accumulate in blood, often causing noticeable symptoms like fatigue, nausea, and swelling.
Patients need specialized care from a nephrologist and should begin preparing for possible kidney failure, including learning about dialysis and transplant options. However, with appropriate treatment, some patients remain in stage 4 for years without progressing to kidney failure.
What are the first signs of kidney problems?
Early kidney problems often produce no obvious signs. When symptoms do appear, they typically include changes in urination (frequency, volume, or appearance), unexplained fatigue, sleep disturbances, dry itchy skin, and mild swelling around eyes or in feet.
Many people discover kidney problems through routine blood or urine tests before experiencing any symptoms. If you have diabetes, high blood pressure, or family history of kidney disease, regular screening catches problems before symptoms develop.
What are 5 foods to avoid for kidney disease?
Five foods to limit or avoid include processed foods high in sodium (frozen dinners, canned soups, deli meats), dark-colored sodas containing phosphate additives, foods high in potassium like bananas and potatoes (when your potassium levels are elevated), whole wheat bread and brown rice in later stages (due to phosphorus content), and star fruit which contains a neurotoxin that healthy kidneys normally eliminate.
However, dietary needs vary significantly between individuals based on disease stage and blood test results. Always work with a renal dietitian for personalized recommendations.
Is chronic kidney disease serious?
Yes, CKD is a serious condition that requires ongoing medical care. It increases risk of cardiovascular disease, can progress to kidney failure requiring dialysis or transplant, and affects multiple body systems. However, serious doesn’t mean hopeless.
Many cases can be prevented, and existing disease can often be slowed or stabilized with appropriate treatment. The key is early detection through screening and diligent management of underlying conditions and risk factors.
What does kidney pain feel like?
Kidney pain typically feels like a deep ache or sharp pain in the back or side, just below the rib cage. It may occur on one or both sides and sometimes radiates toward the abdomen or groin. However, chronic kidney disease usually doesn’t cause kidney pain.
Pain more commonly indicates acute problems like kidney stones, infections, or sudden injury. If you experience severe back or side pain, especially with fever, blood in urine, or difficulty urinating, seek immediate medical attention.
How does kidney disease affect pregnancy?
Kidney disease complicates pregnancy, increasing risks for both mother and baby. Women with CKD face higher rates of preeclampsia (dangerous blood pressure elevation), preterm delivery, low birth weight babies, and worsening kidney function.
However, many women with mild kidney disease successfully carry pregnancies with careful monitoring and management. Advanced kidney disease makes pregnancy riskier and less likely to succeed. Women with kidney disease considering pregnancy should discuss risks and management strategies with both their nephrologist and obstetrician before conceiving.
What are the three early warning signs of a kidney?
Three early warning signs include foamy or bubbly urine (indicating protein loss), changes in urination frequency or volume (especially increased nighttime urination), and swelling around eyes or in hands and feet (from fluid retention).
However, early kidney disease often produces no warning signs at all. This is why screening tests prove more reliable than symptoms for early detection, especially for people with diabetes, high blood pressure, or family history of kidney disease.
How to stop diarrhea in kidney patients?
Managing diarrhea in kidney patients requires addressing the underlying cause, which might include medications (especially phosphate binders or antibiotics), dietary factors, or underlying conditions. Consult your healthcare provider before taking over-the-counter anti-diarrheal medications, as some may not be safe with kidney disease.
Stay hydrated if diarrhea is mild, but avoid excessive fluid intake if you have fluid restrictions. Adjust diet by avoiding trigger foods and eating smaller, frequent meals. Persistent or severe diarrhea requires medical evaluation, especially if accompanied by fever, severe cramping, or blood in stool.
Chronic kidney disease is a journey that requires vigilance, but you do not have to walk it alone. From understanding the basics of chronic kidney disease to navigating the later stages, knowledge is your best defense against kidney failure.
Dr. Prof. Aimun Ahmed is dedicated to providing world-class, compassionate care to help you manage these challenges. Whether you are looking to prevent the disease or need complex care for kidney failure, Dr. Ahmed’s evidence-based approach ensures safety and precision.
If you are concerned about your kidney health or have noticed any symptoms, don’t wait. Early intervention is the key to protecting your body and your future. Reach out today to schedule a consultation and take control of your health.