Your kidneys work silently every day, filtering waste and keeping your body in balance. But what happens when they can’t do their job anymore? For millions of people worldwide, the answer lies in kidney dialysis—a treatment that takes over when kidneys fail. If you’ve recently been told you might need dialysis, you’re probably feeling overwhelmed. Questions flood your mind: Will it hurt? How will it change my life? Can I still work, travel, or enjoy time with family?
Here’s the truth: dialysis isn’t the end of your story. It’s a bridge that helps people live full, meaningful lives even when their kidneys no longer function properly. Whether you’re facing this journey yourself or supporting someone who is, understanding what dialysis really involves can transform fear into confidence. This guide walks you through everything you need to know—from how different types of dialysis work to what daily life looks like for patients. You’ll discover practical insights backed by decades of clinical experience, helping you make informed decisions about your kidney care.
Table of Contents
Understanding Kidney Dialysis
Kidney dialysis is a medical treatment that performs the essential functions your kidneys can no longer handle on their own. When kidneys fail, waste products, excess fluid, and dangerous toxins build up in your blood. Without intervention, this accumulation becomes life-threatening within days.
Dialysis acts as an artificial kidney, removing these harmful substances and maintaining the delicate chemical balance your body needs to survive. The treatment filters your blood through a special membrane, pulling out waste and extra fluid while keeping important nutrients where they belong.
Think of your kidneys as your body’s filtration plant. When this plant shuts down, dialysis becomes the backup system that keeps everything running. It doesn’t cure kidney disease, but it does give people with renal disease the chance to live for years—even decades—while waiting for a transplant or managing chronic conditions.
Most people start dialysis when they reach the last stage of chronic kidney disease, also called end-stage renal disease. At this point, kidneys function at less than 15% of their normal capacity. Your doctor will monitor your kidney function through regular tests and help you prepare before dialysis becomes necessary.
What Are the 4 Types of Dialysis
Dialysis comes in different forms, each suited to different medical needs and lifestyles. Understanding these options helps you and your doctor choose the best approach for your situation.
- Hemodialysis is the most common type. During this procedure, your blood flows through a machine with a special filter called a dialyzer. The machine cleans your blood and returns it to your body. Most people receive hemodialysis at a dialysis center three times weekly, with each session lasting about four hours.
- Peritoneal dialysis uses the lining of your abdomen (called the peritoneum) as a natural filter. A cleansing fluid flows into your belly through a catheter, absorbs waste from your blood, then drains out. Many patients perform this at home, giving them more flexibility and independence.
- Within peritoneal dialysis, there are two main approaches. Continuous Ambulatory Peritoneal Dialysis (CAPD) doesn’t require a machine. You manually exchange the fluid several times throughout the day. Automated Peritoneal Dialysis (APD) uses a machine called a cycler that performs exchanges while you sleep.
- Continuous Renal Replacement Therapy (CRRT) is a fourth type used mainly in hospitals for people with acute kidney disease or those too unstable for standard dialysis. This gentle, round-the-clock treatment slowly removes waste and fluid over 24 hours.
Each type has benefits and considerations. Hemodialysis is proven and reliable but requires multiple weekly visits. Peritoneal dialysis offers freedom but demands daily commitment. Your medical team will help you compare options based on your health, lifestyle, and personal preferences.
Kidney Dialysis Causes
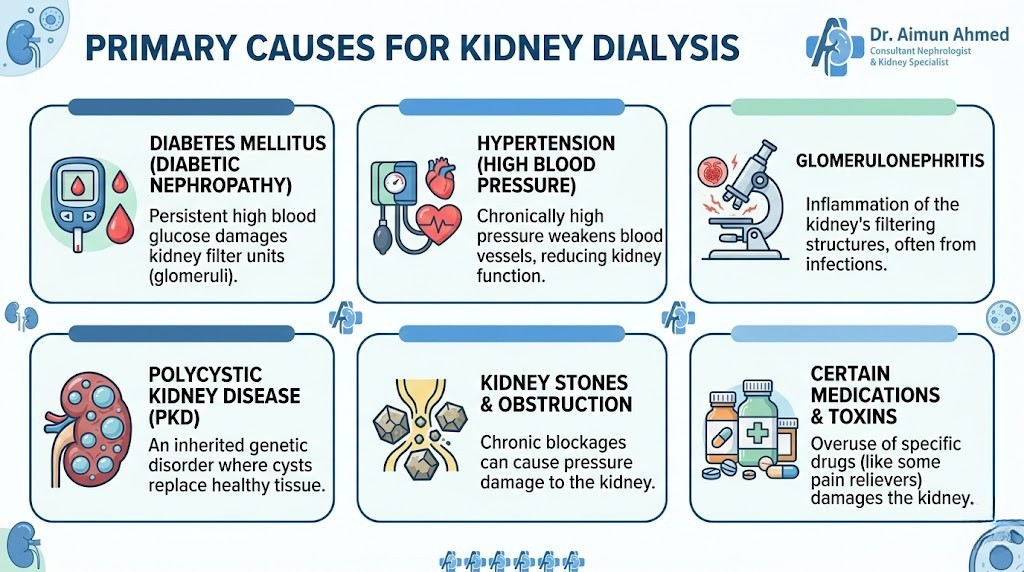
Several conditions can damage your kidneys severely enough to require dialysis. Understanding these causes helps you recognize risk factors and potentially slow disease progression before reaching end-stage kidney failure.
- Diabetes stands as the leading cause of kidney failure worldwide. High blood sugar levels gradually damage the tiny filters in your kidneys called nephrons. This condition, known as diabetic nephropathy, develops slowly over years. Both Type 1 and Type 2 diabetes can lead to this complication if blood sugar isn’t well-controlled.
- High blood pressure ranks as the second most common cause. When blood flows through your kidneys with too much force, it damages the delicate blood vessels. Over time, this reduces the kidneys’ ability to filter waste effectively. Managing blood pressure becomes crucial in protecting kidney function.
- Multiple myeloma and other blood disorders can cause proteins to build up in your kidneys, leading to damage. In some cases, this results in Dialysis-related amyloidosis, where abnormal proteins deposit in tissues and organs.
- Chronic conditions like polycystic kidney disease (where fluid-filled cysts grow in the kidneys), glomerulonephritis (inflammation of the kidney’s filtering units), and recurrent kidney infections can all progress to failure over time.
Acute causes also exist. Sudden blood loss, severe infection, certain medications, or blocked urine flow can cause rapid kidney failure requiring immediate dialysis. Unlike chronic kidney disease, acute kidney injury sometimes reverses with proper treatment.
Kidney Dialysis Symptoms
Recognising when your body signals the need for dialysis can be life-saving. As kidney function declines, symptoms become more apparent and severe.
- Extreme fatigue often appears first. When kidneys fail to remove waste properly, toxins accumulate in your blood, making you feel exhausted no matter how much you rest. This isn’t normal tiredness—it’s a profound lack of energy that interferes with daily activities.
- Swelling becomes noticeable in your legs, ankles, feet, and sometimes your face. Failed kidneys can’t remove excess fluid, which then builds up in your body’s tissues. You might notice your shoes feeling tighter or rings not fitting properly.
- Shortness of breath occurs when fluid accumulates in your lungs or when anemia (low red blood cell count) develops. You may struggle to climb stairs or complete tasks that once felt easy.
- Changes in urination provide clear warning signs. You might urinate much less than normal, or your urine may appear foamy or contain blood. Some people experience the opposite—urinating frequently, especially at night.
- Nausea, vomiting, and loss of appetite happen as waste products build up in your system. Food might taste metallic or simply unappealing. Many patients lose weight unintentionally.
- Itching can become severe and persistent as waste products settle in your skin. Muscle cramps and confusion or difficulty concentrating may also develop.
If you experience multiple symptoms, especially if you have risk factors like diabetes or high blood pressure, contact your doctor immediately. Early intervention can help manage symptoms and prepare you properly for treatment.
Kidney Dialysis Machine
The dialysis machine—often called a hemodialysis machine—is a sophisticated piece of medical equipment that becomes a familiar companion for many patients. Understanding how it works can reduce anxiety about treatment.
The machine contains several key components working together.
- At its heart is the dialyzer, sometimes called an artificial kidney. This hollow tube holds thousands of thin fibers with microscopic pores. Your blood flows through these fibers while a special cleansing solution called dialysate flows around them.
- The blood pump carefully pulls blood from your body through a tube, sends it through the dialyzer at a controlled rate, then returns cleaned blood through another tube. The machine monitors blood flow constantly, ensuring safety throughout the process.
- Monitors and alarms track your blood pressure, temperature, and the composition of your blood and dialysate. If anything falls outside safe parameters, alarms alert the medical staff immediately.
- The dialysate delivery system mixes purified water with concentrated solutions to create the perfect fluid for removing waste. The composition can be adjusted based on your specific needs—more or less of certain minerals, for example.
- Modern machines include touchscreen controls and sophisticated computer systems. They’re much quieter and more efficient than older models. Most patients grow comfortable with the rhythmic sounds and gentle vibrations during treatment.
At dialysis centers, trained nurses and technicians operate these machines, monitor patients, and respond to any issues. The technology has become incredibly reliable, with multiple safety features protecting patients throughout each session.
Kidney Dialysis Procedure
Preparation Phase
Starting dialysis involves several steps, beginning well before your first treatment session. Proper preparation helps ensure the procedure goes smoothly and minimizes complications.
Hemodialysis Access Creation
Creating vascular access comes first for hemodialysis. Your surgeon will create an access point where needles can be inserted to draw and return blood.
- Arteriovenous Fistula (AV Fistula): The most common type is an arteriovenous fistula, where an artery and vein in your arm are surgically connected. This usually needs to mature for several weeks before use.
- AV Graft: Alternatively, doctors might create an AV graft using a synthetic tube to connect an artery and vein.
- Central Venous Catheter: In emergencies, a central venous catheter can be placed in your neck or chest for immediate access, though this is typically temporary.
Peritoneal Dialysis Access
For peritoneal dialysis, a soft catheter is surgically placed in your abdomen. This also needs time to heal before regular use begins.
During a Hemodialysis Session
Getting Started
During a hemodialysis session, you’ll sit in a comfortable chair. A nurse inserts two needles into your access site—one to carry blood to the machine, another to return it. Some patients describe a brief pinch during needle insertion, but most adjust quickly.
During Treatment
As the machine runs, you can read, watch TV, use your phone, or sleep. Most people feel comfortable during treatment, though some experience mild effects like feeling cold or getting muscle cramps.
Monitoring and Safety
The medical team monitors you throughout, checking your blood pressure regularly and adjusting the machine as needed. Removing too much fluid too quickly can cause dizziness or nausea, so technicians carefully control the pace.
After Treatment
After treatment, needles are removed and pressure is applied to prevent bleeding. Most patients feel tired initially but gradually adapt to the routine.
Kidney Dialysis Process
The dialysis process extends beyond the hours spent at a treatment center or performing exchanges at home. It involves continuous attention to diet, medication, and lifestyle.
Pre-Treatment Monitoring
Before treatment, you’ll need blood tests to check your kidney function, electrolyte levels, and other important markers. These tests help your care team adjust your dialysis prescription—determining how long sessions should last and how much fluid to remove.
Weight monitoring happens before and after each session. The difference tells your team how much fluid accumulated and needs to be removed. Staying close to your “dry weight” (your weight without excess fluid) helps you feel better and reduces strain on your heart.
Dietary Management
Dietary management plays a crucial role. When kidneys fail, they can’t eliminate certain minerals and nutrients effectively. You’ll likely need to limit sodium (salt), potassium, and phosphorus in your diet. A renal dietitian will provide guidance on which foods to reduce or avoid.
Protein Balance
Protein needs special attention. While healthy kidneys can handle large amounts of protein, dialysis patients need enough to stay strong but not so much that waste products overwhelm the treatment. Your dietitian will calculate the right balance for you.
Fluid Restrictions
Fluid restrictions often prove challenging. If your kidneys produce little or no urine, drinking too much causes dangerous fluid buildup between sessions. Many patients learn to measure their fluid intake carefully, including liquid in foods like soup and ice cream.
Medication Management
Medications become part of daily routine. You might take medicines to control blood pressure, bind phosphorus from food, treat anemia, or prevent bone disease. Taking these as prescribed significantly improves outcomes.
Kidney Dialysis Side Effects
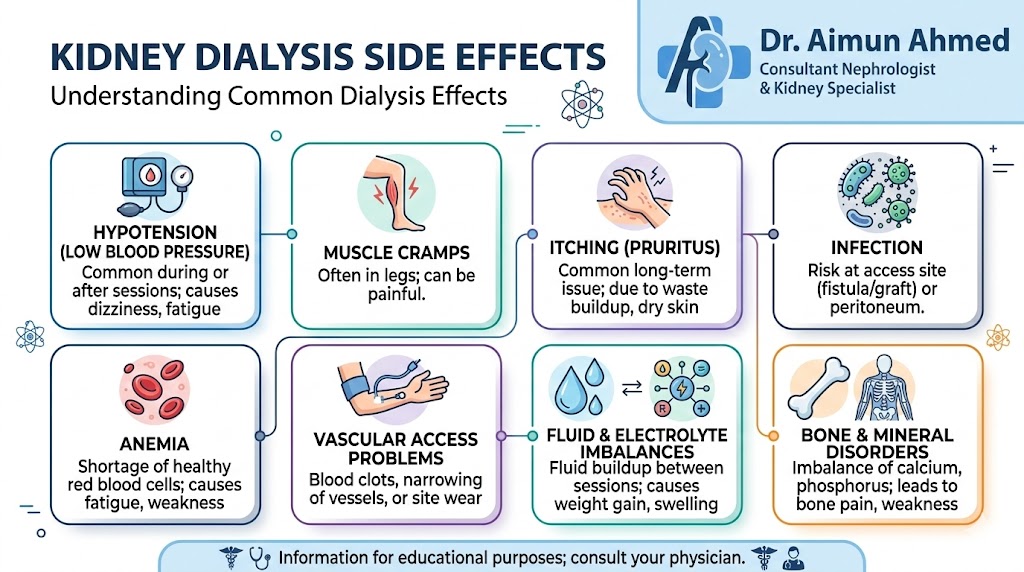
While dialysis saves lives, it can cause side effects. Understanding these helps you recognize normal responses versus problems requiring medical attention.
- Low blood pressure is one of the most common effects during hemodialysis. Removing fluid quickly can cause your blood pressure to drop, leading to dizziness, nausea, or lightheadedness. Your medical team adjusts treatment speed and monitors you carefully to minimize this risk.
- Muscle cramps, particularly in your legs, often occur toward the end of sessions. These painful spasms result from rapid fluid and electrolyte changes. Adjusting your dry weight or dialysate composition usually helps.
- Fatigue after treatment is normal, though it typically improves as your body adjusts to the routine. Some people feel energized after dialysis, while others need rest.
- Itching troubles many patients, caused by phosphorus buildup or dry skin. Using moisturizer, taking prescribed phosphate binders, and following dietary guidelines can reduce this symptom.
- Sleep problems affect numerous patients, including restless legs syndrome and sleep apnea. Discuss these with your doctor, as treatments exist to improve sleep quality.
- Infection remains a serious concern. Access sites for hemodialysis or peritoneal dialysis catheters can become infected if not properly cared for. Following cleaning instructions precisely and watching for signs of infection (redness, warmth, discharge, fever) is essential.
- Dialysis-related amyloidosis can develop in long-term patients when a protein called beta-2-microglobulin builds up, forming deposits in joints and tissues. This causes pain and stiffness, particularly in shoulders, hands, and knees.
- Anemia commonly develops because damaged kidneys don’t produce enough erythropoietin, a hormone that stimulates red blood cell production. Medications can treat this effectively.
Most side effects can be managed or reduced through adjustments in treatment, medication, or diet. Never hesitate to report symptoms to your care team.
What Causes Kidney Failure
Kidney failure doesn’t happen overnight—it’s typically the end result of long-term damage from various conditions. Understanding these causes empowers you to protect your kidneys or slow disease progression.
- Diabetic nephropathy damages kidneys through consistently high blood sugar levels. Excess glucose in your blood injures the tiny filtering units in your kidneys. Over years or decades, this damage accumulates until kidneys can no longer function properly. Managing diabetes through diet, exercise, and medication significantly reduces this risk.
- Hypertensive nephrosclerosis occurs when chronic high blood pressure damages kidney blood vessels. The pressure literally wears out the delicate vessels that filter your blood. Controlling blood pressure protects not just your kidneys but also your heart and brain.
- Glomerular diseases affect the glomeruli—clusters of tiny blood vessels that do the actual filtering work. Conditions like glomerulonephritis cause inflammation and damage to these structures. Some forms are genetic, while others result from infections or autoimmune diseases.
- Polycystic kidney disease is an inherited condition where cysts grow in the kidneys, eventually interfering with function. While you can’t prevent genetic diseases, managing blood pressure and treating infections promptly can slow progression.
- Chronic urinary tract problems like recurrent infections, kidney stones, or structural abnormalities can cause permanent kidney damage over time. Treating infections promptly and addressing underlying issues helps protect kidney function.
- Toxins and medications sometimes harm kidneys. Certain pain relievers (especially NSAIDs like ibuprofen when used long-term), some antibiotics, and contrast dyes used in imaging tests can damage kidneys, particularly if you already have reduced kidney function.
- Acute causes include sudden events like severe bleeding, heart attack, liver failure, severe dehydration, or obstruction of urine flow. These can cause rapid kidney failure requiring emergency dialysis.
What Causes Kidney Disease
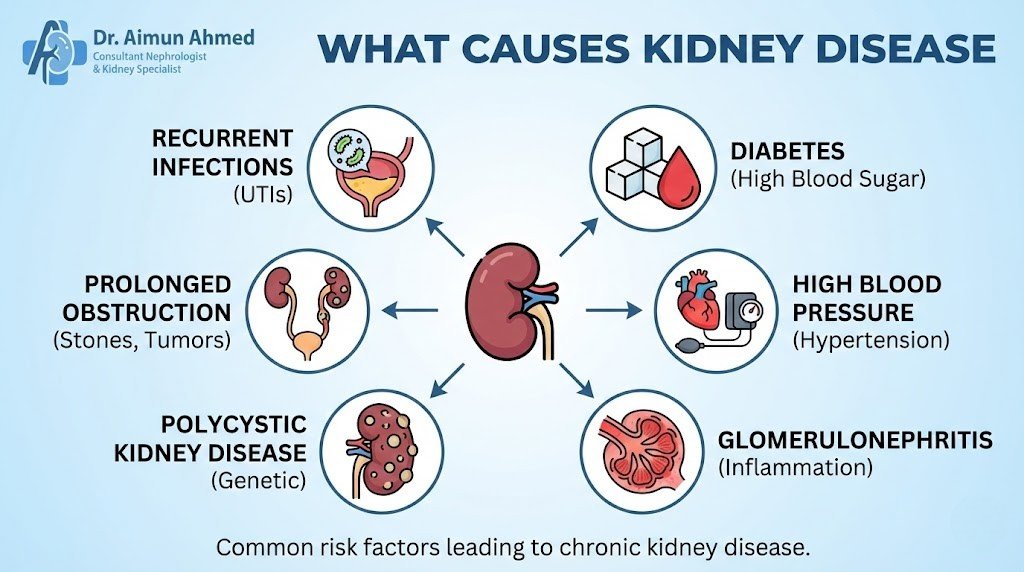
Kidney disease encompasses a spectrum from mild dysfunction to complete failure. Many factors contribute to its development, and understanding them helps with prevention and early intervention.
- Metabolic conditions beyond diabetes and hypertension also affect kidneys. Obesity increases risk significantly, both directly through metabolic changes and indirectly by promoting diabetes and high blood pressure. Managing weight through healthy eating and regular activity protects kidney function.
- Cardiovascular disease and kidney disease often occur together. They share risk factors and each condition worsens the other. What’s bad for your heart is usually bad for your kidneys too.
- Autoimmune diseases like lupus can attack the kidneys as part of their systemic effects. Lupus nephritis requires specific treatment to prevent permanent damage.
- Genetic factors play a role in many kidney diseases. If close family members have kidney disease, your risk increases. Genetic testing and early screening can help identify problems before they progress.
- Age naturally affects kidney function—most people experience some decline after age 40. This normal aging makes kidneys more vulnerable to other risk factors.
- Smoking damages blood vessels throughout your body, including those in your kidneys. It also accelerates progression of existing kidney disease. Quitting smoking is one of the most important steps you can take to protect kidney health.
- Certain infections, particularly repeated urinary tract infections or specific viral infections like hepatitis, can lead to chronic kidney damage if not properly treated.
- Environmental exposures to heavy metals, certain chemicals, or contaminated water can harm kidneys over time. Occupational safety measures and awareness of environmental risks matter.
Diagnosis of Chronic Kidney Disease
Early detection of chronic kidney disease saves lives and can slow progression dramatically. Diagnosis involves several tests that paint a complete picture of kidney function.
- Blood tests measure key indicators. The most important is creatinine, a waste product that healthy kidneys filter out efficiently. Your doctor uses creatinine levels to calculate your estimated glomerular filtration rate (eGFR) essentially a measure of how well your kidneys filter blood. An eGFR below 60 for three months indicates chronic kidney disease.
- Blood urea nitrogen (BUN) is another waste product that accumulates when kidneys fail. High BUN levels suggest reduced kidney function.
- Electrolyte tests check levels of sodium, potassium, and phosphorus. Imbalances in these minerals can indicate kidney problems and cause serious complications if not addressed.
- Urine tests provide crucial information. Albumin is a protein that shouldn’t appear in urine—its presence suggests kidney damage. Even small amounts (microalbuminuria) can signal early disease, particularly in people with diabetes or hypertension.
- Urine creatinine measurements help assess how much your kidneys filter. The albumin-to-creatinine ratio combines these measurements for a clearer picture of kidney health.
- Imaging tests like ultrasounds, CT scans, or MRIs show kidney structure. They can identify cysts, tumors, stones, or blockages. Ultrasound is often first because it’s safe, painless, and provides good information about kidney size and structure.
- Kidney biopsy involves taking a small tissue sample for examination under a microscope. This isn’t needed for everyone but can help diagnose specific types of kidney disease or guide treatment decisions.
- Staging ranges from 1 to 5 based on eGFR. Stage 1 represents mild damage with normal or high filtration, while stage 5 (eGFR below 15) indicates kidney failure requiring dialysis or transplant.
Regular screening is vital if you have diabetes, high blood pressure, heart disease, or family history of kidney disease. Catching problems early allows intervention before permanent damage occurs.
Function of Kidney
Your kidneys do far more than most people realize. These fist-sized organs perform complex tasks essential for life, which is why their failure affects your entire body.
- Filtering waste is the function everyone knows about. Every day, your kidneys process about 200 quarts of blood, removing waste products and excess substances while keeping what you need. These waste products come from normal muscle activity, food breakdown, and cell metabolism. Without filtration, these toxins accumulate to dangerous levels within days.
- Regulating fluid balance keeps your body from becoming waterlogged or dehydrated. Your kidneys adjust how much water they excrete based on what you drink and what your body needs. This regulation affects blood volume and blood pressure.
- Maintaining electrolyte balance ensures proper nerve and muscle function. Your kidneys carefully control levels of sodium, potassium, calcium, phosphorus, and other minerals. Too much or too little of these can cause serious problems—from irregular heartbeats to seizures.
- Controlling blood pressure involves multiple kidney functions. They regulate blood volume, produce renin (a hormone affecting blood pressure), and control sodium balance—all crucial for maintaining healthy blood pressure.
- Producing hormones extends kidney function beyond filtration. They make erythropoietin, which stimulates red blood cell production. This is why kidney disease often causes anemia. They also produce calcitriol, the active form of vitamin D, which helps your body absorb calcium and maintain bone health.
- Balancing acid levels in your blood (pH balance) is another critical job. Your kidneys remove excess acid and maintain the narrow pH range your body needs to function properly.
When kidneys fail, all these functions stop working properly. Dialysis takes over the waste removal and fluid balance functions, but can’t replicate everything kidneys do. This is why transplant offers the most complete solution when possible.
Acute Kidney Disease
Acute kidney disease (also called acute kidney injury or AKI) differs significantly from chronic kidney disease. It develops suddenly—sometimes within hours or days—rather than gradually over years.
- Causes of acute kidney disease include severe infections (sepsis), major surgery, heart attack, severe dehydration, certain medications, contrast dyes, severe bleeding, or anything that suddenly reduces blood flow to the kidneys. Blocked urine flow from kidney stones, tumors, or enlarged prostate can also cause acute failure.
- Symptoms appear quickly and can include decreased urine output, swelling from fluid retention, shortness of breath, confusion, nausea, chest pain or pressure, and in severe cases, seizures or coma.
- Diagnosis involves the same tests used for chronic disease—blood tests for creatinine and BUN, urine tests, and imaging—but doctors look for rapid changes in these values rather than gradual decline.
- Treatment focuses on addressing the underlying cause. If severe infection caused it, antibiotics are crucial. If medications triggered it, stopping them may help. If dehydration is the culprit, fluids can restore function.
Many patients need temporary dialysis to remove waste and fluid while kidneys recover. Unlike chronic kidney disease, acute kidney injury often reverses if caught and treated quickly. Many people recover full or partial kidney function.
However, acute kidney disease can also progress to chronic kidney disease, especially if the injury was severe or if underlying conditions (like diabetes) exist. Close monitoring after recovery is essential.
Prevention involves staying well-hydrated (especially during illness or hot weather), using medications as directed, managing chronic conditions carefully, and seeking prompt treatment for infections or injuries.
How to Avoid Dialysis
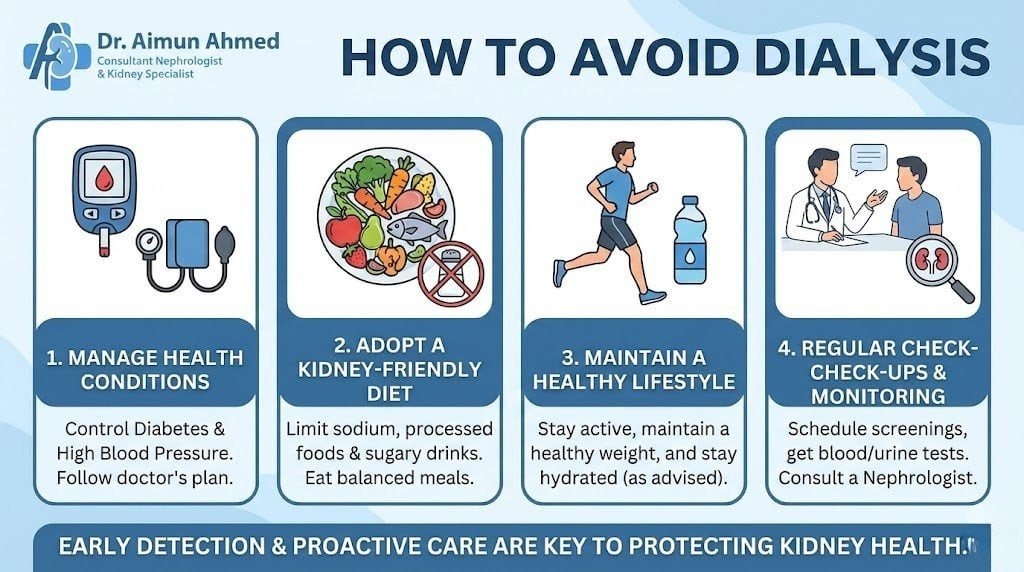
While not everyone can prevent kidney disease, many people can slow its progression and potentially avoid dialysis altogether through proactive health management.
- Control blood sugar if you have diabetes. Keeping hemoglobin A1C below 7% (or your doctor’s target) significantly reduces kidney damage risk. Monitor blood sugar regularly, take medications as prescribed, and work with your healthcare team to optimize management.
- Manage blood pressure aggressively. Target levels are typically below 130/80 mm Hg, though your doctor might recommend different goals based on your situation. ACE inhibitors and ARBs (types of blood pressure medications) not only lower blood pressure but also provide specific kidney protection.
- Follow a kidney-friendly diet even before disease reaches advanced stages. Reduce sodium, which raises blood pressure and strains kidneys. Limit protein to recommended levels—too much forces kidneys to work harder. Your doctor or dietitian can provide personalized guidelines.
- Stay active through regular exercise. Physical activity helps control blood pressure, blood sugar, and weight—all protective factors for kidneys. Aim for at least 150 minutes of moderate activity weekly unless your doctor advises otherwise.
- Maintain a healthy weight. Obesity increases risk of diabetes, hypertension, and direct kidney damage. Even modest weight loss can improve kidney function and slow disease progression.
- Quit smoking. Tobacco damages blood vessels, accelerates kidney disease progression, and reduces effectiveness of blood pressure medications. Quitting provides one of the most powerful protective effects you can achieve.
- Stay hydrated with water, not sugary drinks. Adequate hydration helps kidneys function optimally, though if you have advanced disease, your doctor may recommend fluid limits.
- Avoid nephrotoxic substances. Use NSAIDs (ibuprofen, naproxen) sparingly and only as directed. Avoid herbal supplements without doctor approval—some harm kidneys. If you need contrast dyes for imaging, ensure you’re well-hydrated and discuss kidney protection strategies with your doctor.
- Treat infections promptly, especially urinary tract infections. Untreated infections can damage kidneys permanently.
- Monitor kidney function regularly if you have risk factors. Early detection allows intervention before irreversible damage occurs. Ask your doctor about appropriate testing frequency.
- Manage underlying conditions. If you have lupus, gout, polycystic kidney disease, or other conditions affecting kidneys, work closely with specialists to optimize treatment.
Remember that chronic kidney disease has five stages. Dialysis typically becomes necessary only at stage 5. Many people live for years—even decades—with stages 1-4 disease through careful management. The earlier you start protecting your kidneys, the better your chances of avoiding dialysis.
Frequently Asked Questions
Is dialysis expensive?
The treatment itself carries significant costs, including the equipment, supplies, medications, and medical staff needed. However, most patients don’t bear these costs directly. In many countries, including the UK, dialysis is covered by national health services.
In the United States, Medicare covers dialysis for most patients regardless of age through the End-Stage Renal Disease program. Private insurance also typically covers treatment. Talk with your dialysis center’s financial counselor about coverage in your specific situation—they can help navigate insurance and identify assistance programs if needed.
Can kidney dialysis be painful?
The procedure itself typically isn’t painful, though some aspects can be uncomfortable. During hemodialysis, needle insertion causes a brief pinch similar to blood draws. Some patients feel cold during treatment or experience muscle cramps as fluid is removed. Peritoneal dialysis generally causes less discomfort, though you might feel pressure when fluid is in your abdomen. Most pain associated with dialysis comes from complications like infections at access sites rather than the treatment itself. Good access care and proper technique minimize discomfort significantly.
How long does kidney dialysis take?
Hemodialysis sessions typically last three to five hours, and most patients need treatment three times weekly. That’s 9-15 hours weekly at a dialysis center. Peritoneal dialysis takes less time per exchange (20-40 minutes) but requires multiple daily exchanges or overnight treatment with a cycler machine. The total time commitment depends on which type you choose and your specific prescription. Your schedule can sometimes be adjusted around work, school, or other commitments by choosing different session times or treatment modalities.
What is the last stage of kidney dialysis?
This question likely refers to end-stage renal disease, the condition requiring dialysis rather than stages of dialysis itself. End-stage renal disease (stage 5 chronic kidney disease) occurs when kidneys function at less than 15% of normal capacity. At this point, dialysis or transplant becomes necessary for survival. Once on dialysis, there aren’t really “stages” of the treatment itself—patients continue dialysis until they receive a transplant or, in some cases, choose to stop treatment.
Can a person survive after kidney dialysis?
Absolutely. Many people live for years or decades on dialysis. Survival depends on multiple factors including age, overall health, underlying conditions, how well you follow treatment recommendations, and diet adherence. Younger patients without other serious health problems often do very well. Older patients with diabetes, heart disease, or other complications face more challenges but can still enjoy meaningful, productive lives. Quality of life on dialysis has improved tremendously with modern technology and treatment approaches. Some patients work full-time, travel, and maintain active social lives while on dialysis.
What happens on the first day of dialysis?
Your first session usually runs shorter than regular treatments—often two to three hours instead of four—to let your body adjust gradually. The medical team will explain each step, answer questions, and monitor you closely. They’ll check your vital signs frequently. You might feel anxious, but nurses are experienced at helping new patients feel comfortable. Some people feel tired afterward, while others feel better than they have in weeks because accumulated toxins are finally being removed. It’s normal to feel emotional—starting dialysis represents a major life change. Bring items to help you relax: a book, tablet, headphones, or a friend for support.
Can you live a normal life on kidney dialysis?
Life with dialysis is different from life without it, but many patients maintain fulfilling, active lives. You’ll need to schedule treatment sessions, follow dietary restrictions, and take medications regularly. However, people on dialysis work, attend school, travel (with planning), enjoy hobbies, and maintain relationships. The key is finding a treatment schedule and modality that fits your lifestyle. Peritoneal dialysis at home offers more flexibility for some people. Home hemodialysis provides another option for independence. The definition of “normal” varies, but with support and adaptation, most patients find their new normal includes much of what matters most to them.
What are the side effects of kidney dialysis?
Common side effects include low blood pressure during treatment, muscle cramps, fatigue, itching, sleep disturbances, and changes in appetite. Some patients develop anemia or bone disease, though medications can manage these. Access site infections remain a concern requiring careful hygiene. Long-term dialysis can lead to Dialysis-related amyloidosis, causing joint pain and stiffness. However, many side effects can be minimized through proper technique, medication adjustments, dietary management, and communication with your care team. Most patients adjust to treatment over time, and side effects often decrease as you and your team fine-tune your dialysis prescription.
Can kidneys start working again after dialysis?
In cases of acute kidney injury, yes—kidneys often recover function after temporary dialysis. The recovery period varies from days to months depending on what caused the injury and how severe it was. However, in chronic kidney disease that has progressed to end-stage renal disease, kidneys almost never recover function.
The damage is permanent. Very rarely, kidney function might stabilize at low levels, potentially allowing reduced dialysis, but complete recovery from end-stage chronic kidney disease is exceptionally uncommon. This is why transplant becomes the goal for many patients—it offers the best chance at life without dialysis.
How many hours of sleep should a dialysis patient get?
Dialysis patients should aim for 7-9 hours of sleep nightly, just like anyone else. However, sleep problems are extremely common in this population. Restless legs syndrome, sleep apnea, and disrupted sleep patterns affect many patients. Poor sleep quality can worsen other symptoms and affect overall health. If you’re struggling with sleep, discuss it with your nephrologist.
Treatments exist for restless legs syndrome and sleep apnea. Adjusting dialysis schedules, reviewing medications, or addressing anemia might also improve sleep quality. Good sleep hygiene—maintaining consistent bedtimes, avoiding screens before sleep, and creating a comfortable sleep environment—helps too.
What is the life expectancy of a person on kidney dialysis?
Life expectancy varies widely based on multiple factors. Age at dialysis starts significantly impacts survival—younger patients typically live longer. Overall health, particularly the presence of diabetes, heart disease, or other conditions, affects longevity. Adherence to treatment, diet, and medication matters enormously.
On average, a 40-year-old starting dialysis might live 10-20+ years, while an 80-year-old might survive 2-5 years. However, these are generalizations—individual experiences vary tremendously. Many patients live well beyond average expectations through excellent self-care and medical management. Quality of life matters as much as length of life, and modern dialysis enables many patients to live meaningful, productive years.
Conclusion
Kidney dialysis is a journey, not just a procedure. It requires resilience, discipline, and a trusted medical partner. Dr. Aimun Ahmed offers the expertise and compassionate care necessary to navigate this path safely. Whether you are exploring options for the first time or seeking to improve your current management plan, discover how world-class nephrology care can transform your experience.
Contact Dr. Aimun Ahmed today to discuss your kidney health and ensure you are receiving the best possible care for your future.