Have you noticed swelling in your face or ankles, or blood in your urine? These could be signs of glomerulonephritis.
Left untreated, this type of kidney inflammation can progress to kidney failure, affecting your ability to filter waste from your blood.
Early diagnosis and proper management can protect your kidneys and preserve their function for years to come.
When your kidneys stop working properly, it can feel frightening and overwhelming. Your kidneys contain tiny blood filters called glomeruli that clean your blood every single day. When these filters become inflamed, a condition develops that affects how your body removes waste and excess fluid.
This guide breaks down everything you need to know about this kind of kidney disease. You’ll learn what happens inside your kidneys, how to recognize warning signs, and what treatment options can help protect your kidney health. Whether you’re experiencing symptoms or supporting someone who is, understanding this condition is the first step toward better kidney care.
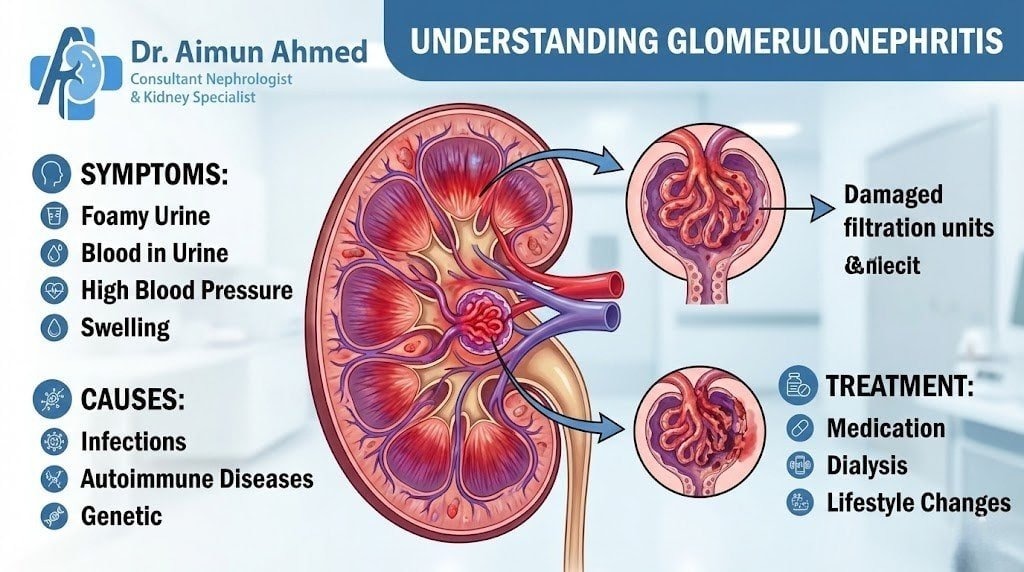
What is Glomerulonephritis?
Glomerulonephritis represents a type of kidney inflammation targeting the glomeruli—microscopic filtering units where blood passes through to remove waste and excess fluid. Think of glomeruli as tiny sieves, with each kidney containing roughly one million of these essential filters. When inflammation strikes, these structures struggle to perform their job effectively.
The condition can appear suddenly (acute) or develop gradually over months or years (chronic glomerulonephritis). In healthy kidneys, the fenestrated endothelium forms a critical barrier within glomeruli, working alongside specialized cells and the glomerular basement membrane (GBM) to prevent protein and red blood cells from leaking into urine. When glomerulonephritis develops, this sophisticated filtering system becomes compromised.
Understanding Glomerulonephritis Symptoms
Symptoms vary dramatically depending on whether the illness develops quickly (acute) or slowly (chronic).
Acute Presentation
When inflammation appears suddenly, patients often notice:
- Dark or rust-colored urine resembling cola
- Foamy urine from excess protein
- Facial puffiness, especially upon waking
- Decreased urine output
- Fatigue and general malaise
Chronic Development
Chronic glomerulonephritis may cause subtle, barely noticeable changes initially. As months pass, symptoms gradually emerge:
- Persistent high blood pressure resistant to treatment
- Steady decline in kidney function detected through blood tests
- Progressive swelling in legs and ankles
- Increasing proteinuria
- Eventually, symptoms of kidney failure if untreated
Some patients experience no symptoms at all during early stages. Routine check-ups may reveal abnormalities before any discomfort begins, highlighting why regular health screenings matter.
Glomerulonephritis Symptoms in Children
Pediatric cases often follow a different pattern. Children typically develop acute glomerulonephritis after streptococcal infections, such as strep throat or skin infections. Parents might notice their child experiencing:
- Sudden puffiness around the eyes, especially upon waking
- Swelling in legs and feet
- Dark or tea-colored urine
- Decreased urination
- Irritability or fatigue
- Stomach pain
Post-streptococcal glomerulonephritis usually resolves with supportive treatment, though careful monitoring ensures complete recovery. Any child showing these symptoms after a recent illness requires prompt medical evaluation to prevent complications.
Types of Glomerulonephritis
Understanding different types helps patients grasp their specific situation better.
Primary Forms
Primary types originate within the kidneys themselves:
- IgA Nephropathy (IgAN): The most common primary glomerulonephritis worldwide, characterized by IgA antibody deposits in glomeruli. This represents what many recent Kidney International study findings focus on, as researchers work to improve outcomes.
- Membranoproliferative Glomerulonephritis: A rare glomerulopathy involving thickening of the glomerular basement membrane and proliferation of cells.
- Minimal Change Disease: More common in children, causing significant protein loss but typically responding well to treatments like prednisone.
Secondary Forms
Secondary types result from systemic diseases affecting multiple body organs:
- Lupus Nephritis: Occurs in patients with systemic lupus erythematosus, an autoimmune condition. The immune system mistakenly attacks healthy tissues, including kidneys.
- Post-Infectious: Develops after bacterial, viral, or parasitic infections. SARS-CoV-2 (COVID-19) has emerged as a trigger in some cases.
- Vasculitis-Related: Associated with inflammation of blood vessels throughout the body.
Each type demands specific management approaches, which is why accurate diagnosis through biopsy and clinical correlation proves essential.
What Causes Glomerulonephritis?
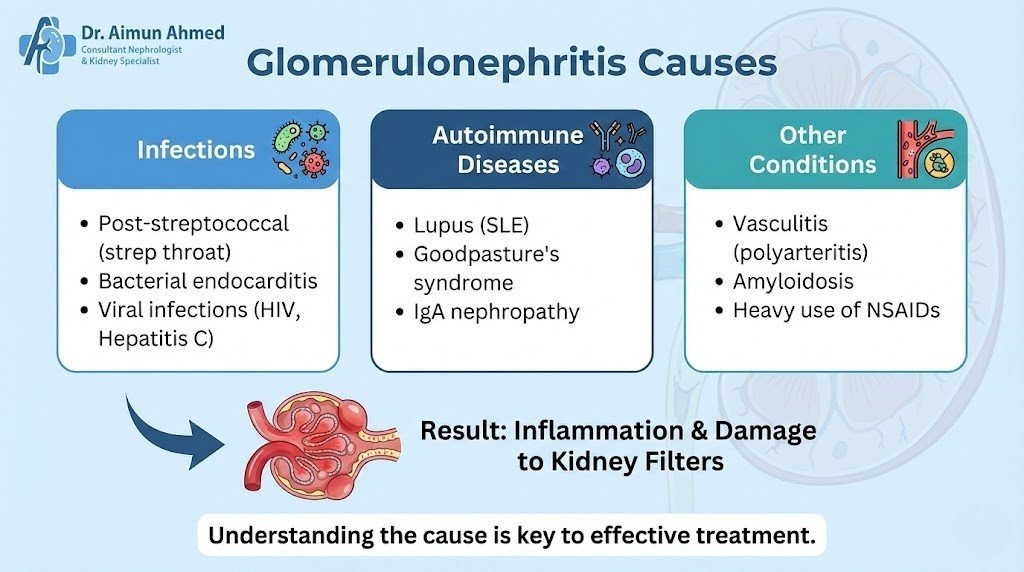
Multiple factors can trigger inflammation in the kidneys filters. Understanding these causes helps in both prevention and treatment approaches.
- Infections – Bacterial infections like strep throat can provoke an immune response that affects the kidneys. Viral infections, including hepatitis B, hepatitis C, and HIV, may also lead to kidney inflammation.
- Immune system disorders – Lupus, a multisystem autoimmune disease, frequently involves the kidneys. The immune system mistakenly attacks healthy tissue, including the glomerular filters.
- Medications and toxins – Certain medications and toxins can damage the small blood vessels in the kidneys.
- Chronic conditions – High blood pressure and diabetes may cause glomerular damage over time.
- Genetic factors – Influence susceptibility in some cases, particularly with conditions that run in families.
- Idiopathic causes – Sometimes, despite thorough testing, the cause remains unknown.
Glomerulonephritis Rash and Related Symptoms
While primarily a kidney disorder, glomerulonephritis can manifest with skin changes in certain cases. These visible signs often provide important diagnostic clues.
Some people develop purpura, which appears as small purple or red spots on the skin. These occur when inflamed blood vessels leak red blood cells under the skin surface. This rash typically appears on the legs and buttocks but can affect other body areas.
IgA vasculitis, formerly called Henoch-Schonlein purpura, commonly produces this type of rash alongside kidney involvement. The combination of skin changes and kidney inflammation helps physicians diagnose this specific condition.
Lupus-related kidney inflammation may coincide with the characteristic butterfly-shaped facial rash. Not everyone with glomerulonephritis develops a rash, but when present, it warrants immediate medical evaluation.
Glomerulonephritis Diagnosis
Accurate diagnosis requires multiple tests to assess kidney function and identify the specific type of inflammation. Your healthcare provider will start with a detailed medical history and physical examination.
Urine Tests
Urine tests form the foundation of diagnosis. A simple urinalysis can detect blood, protein, and cellular debris that should not be present. A 24-hour urine collection measures exactly how much protein your kidneys are losing.
Blood Tests
Blood tests evaluate kidney function and search for underlying causes:
- Anti-GBM antibodies
- Complete blood count
- Creatinine and blood urea nitrogen levels
- Tests for antibodies and complement levels
Kidney Biopsy
A kidney biopsy provides definitive diagnosis in many cases. This procedure remains the gold standard for acute glomerulonephritis diagnosis when the type of inflammation is unclear or when treatment decisions require precise information.
Understanding Glomerulonephritis Complications
Without proper management, this condition can lead to serious long-term complications affecting overall health and quality of life.
Kidney Failure
Progressive damage to filtering units may eventually result in chronic kidney disease or even end-stage renal failure requiring dialysis or transplantation. Prof. Ahmed’s three decades of clinical practice demonstrate that early intervention significantly reduces this risk.
Cardiovascular Problems
Persistent hypertension damages blood vessels and increases heart disease risk. Fluid retention strains the cardiovascular system, potentially causing heart failure.
Acute Complications
Sudden severe inflammation can trigger acute kidney injury, requiring immediate hospitalization. Dangerous electrolyte imbalances, particularly elevated potassium levels, may affect heart rhythm. Pulmonary edema (fluid in lungs) from poor fluid regulation creates breathing difficulties.
Chronic Health Impact
Long-term protein loss weakens immune function and affects nutrition. Bone health deteriorates when kidneys cannot properly balance minerals. Anemia develops as damaged kidneys produce insufficient erythropoietin, the hormone stimulating red blood cell production.
Prevention through proper treatment remains far superior to managing complications later.
Treatment of Glomerulonephritis

Treatment approaches depend on the type, severity, and underlying cause of inflammation. The goals focus on reducing inflammation, managing symptoms, slowing disease progression, and preventing complications.
Main Treatment Approaches:
- Blood Pressure Management – ACE inhibitors or ARBs help control hypertension while reducing protein loss
- Diuretics – Help reduce swelling by removing excess fluid from the body
- Immunosuppressive Medications – Corticosteroids and other immune-suppressing drugs
- Antibiotics – Treat bacterial infections that trigger certain types of kidney inflammation
- Dietary Changes – Reducing salt intake and protein restriction when needed
- Dialysis – For acute cases with severe kidney failure
Glomerulonephritis Radiology and Imaging
While kidney biopsy provides the most detailed information, imaging studies play an important supporting role in diagnosis and monitoring.
- Ultrasound – Most common imaging technique showing kidney size and structure
- CT Scans – Provide more detailed images to rule out other kidney problems
- MRI – Offers excellent soft tissue detail without radiation exposure
- Nuclear Medicine Scans – Measure kidney function using radioactive tracers
Living with Glomerulonephritis: Long-term Management
- Many people successfully manage this condition with proper care and lifestyle adjustments.
- Lifestyle modifications – healthy weight, physical activity, no smoking
- Regular medical follow-up with nephrologist
- Emotional support and counseling
- Medication adherence
- Infection prevention
- Symptom monitoring
Frequently Asked Questions About Glomerulonephritis
What are the three types of glomerulonephritis?
While many specific forms exist, three major categories include acute glomerulonephritis (sudden onset, often infection-related), chronic glomerulonephritis (gradual progression over years), and rapidly progressive glomerulonephritis (aggressive form causing swift kidney damage). Each category encompasses several distinct subtypes diagnosed through biopsy and laboratory testing.
What is the triad of glomerulonephritis?
The classic triad consists of hematuria (blood in urine), proteinuria (protein in urine), and edema (swelling). These three signs together strongly suggest glomerular inflammation. However, not all patients present with all three features, and their presence and severity vary depending on the specific type and stage of the condition.
What is the most common cause of acute glomerulonephritis?
Post-streptococcal glomerulonephritis represents the most common cause of acute glomerulonephritis worldwide. This typically develops one to two weeks after a strep throat or skin infection. The immune response to the bacterial infection triggers kidney inflammation. Children are particularly susceptible, though adults can develop it too.
What does glomerulonephritis feel like?
Many people experience fatigue and general unwellness. You might notice puffiness around your eyes or swollen ankles. Some describe a feeling of abdominal fullness or mild discomfort in the lower back. Others feel no symptoms at all, especially in mild cases. Symptoms vary greatly depending on the type and severity of inflammation.
What are the first signs of glomerulonephritis?
Often, the earliest signs include changes in urine appearance such as pink, red, or cola-colored urine from blood. Foamy urine from excess protein may be noticeable. Facial puffiness, especially upon waking, commonly appears early. Some people first discover the condition through routine blood or urine tests before symptoms develop.
What is the most common primary glomerulonephritis?
IgA nephritis holds this distinction globally. This condition occurs when IgA antibodies accumulate in the glomeruli, causing inflammation. It often presents with visible blood in the urine during or shortly after upper respiratory infections. While some cases remain mild, others progress to chronic kidney disease requiring long-term management.
What is the gold standard for acute glomerulonephritis?
Kidney biopsy remains the gold standard for definitive diagnosis. This procedure involves removing a small kidney tissue sample for microscopic examination. The biopsy reveals the specific type of inflammation, extent of damage, and whether scarring has occurred. This information guides treatment decisions and helps predict outcomes.
What are three risk factors for glomerulonephritis?
Having autoimmune diseases like lupus significantly increases risk. A history of certain infections, particularly strep throat or hepatitis, raises susceptibility. Family history of kidney disease or glomerulonephritis suggests genetic predisposition. Other factors include uncontrolled hypertension, diabetes, and exposure to certain medications or toxins.
What is the main treatment for glomerulonephritis?
Treatment varies by type and cause but typically focuses on controlling blood pressure, reducing inflammation, and managing symptoms. Medications like ACE inhibitors or ARBs protect kidney function. Immunosuppressive drugs may be necessary for immune-mediated types. Treating underlying conditions, dietary modifications, and regular monitoring form essential components of comprehensive management.
What blood test will confirm glomerulonephritis?
No single blood test confirms the diagnosis. Rather, a combination of tests suggests kidney inflammation. Elevated creatinine and blood urea nitrogen indicate impaired kidney function. Complete blood count may show anemia. Tests for specific antibodies, complement levels, and anti-GBM antibodies help identify the type. These results, combined with urine tests, guide further diagnostic steps.
Expert Kidney Care with Prof. Aimun Ahmed
Understanding glomerulonephritis empowers you to recognize symptoms early and seek appropriate care. Whether you are dealing with acute inflammation or managing chronic kidney disease, expert guidance makes a significant difference in outcomes.
Prof. Aimun Ahmed brings over three decades of specialized experience to kidney care. As a Consultant Nephrologist at Lancashire Teaching Hospitals, he has successfully managed more than 5,000 patients with complex kidney conditions. His expertise spans Chronic Kidney Disease, Transplant Medicine, and Hypertension management.
Prof. Ahmed approach combines evidence-based medicine with compassionate, personalized care. He believes in clear communication, helping patients understand their condition and treatment options fully. His commitment to safety and precision ensures the highest quality kidney care available.
If you are experiencing symptoms of kidney inflammation or have been diagnosed with glomerulonephritis, professional evaluation and treatment can protect your kidney function and improve your quality of life. Early intervention offers the best chance for favorable outcomes.
MEDICAL DISCLAIMER
This article provides educational information about glomerulonephritis. It does not constitute medical advice and should not replace consultation with qualified healthcare professionals. If you are experiencing symptoms of kidney disease, please seek evaluation from a nephrologist or your healthcare provider.